| Interview Fayaz A. Shawl, M.D. |
||
| |
|
|
 |
Fayaz
A. Shawl, M.D. is Director of Interventional Cardiology at
Washington Adventist Hospital in Takoma Park, Maryland, and
at Prince George's Hospital Center. He is also Clinical Professor
of Medicine at George Washington University Medical School.
In the early days of angioplasty, Dr. (then Maj.) Shawl brought
the U.S. military into the balloon age when he performed the
first PTCA at a military hospital (Walter Reed). |
|
|
A pioneer in interventional cardiology, Dr. Shawl trained under Andreas Gruentzig and Richard Myler. He has been teaching through live demonstration courses since 1988, and has personally disseminated the technique throughout the world. Having performed over 11,000 interventional procedures, Dr. Shawl has been an innovator in the use of Percutaneous Cardiopulmonary Bypass Support (PCPS) for high-risk angioplasty, and he continues working on such new technologies as Percutaneous Transmyocardial Revascularization (PTMR -- sometimes called PMR), hybrid MIDCAB procedures and carotid stenting. All of these techniques will be demonstrated live at his upcoming Tenth Annual Live Demonstration Course on May 1-4, 1998, and are also discussed in this interview. |
 Dr. Shawl's Tenth Annual Live Demonstration Course will be held May 1-4, 1998 in Washington, DC |
|
 Q:
What is "high risk angioplasty"? Q:
What is "high risk angioplasty"? Dr. Shawl: High-risk angioplasty means angioplasty in patients who have poor LV function alone or with other medical conditions that make them a high risk candidate for angioplasty or even bypass surgery. We mean people who have had previous multiple myocardial infarctions with multiple coronary stenoses. Or they have only one open artery which is also threatening to close. In these high risk patients, one cannot perform angioplasty or any other intervention because their heart will not tolerate the procedure. But with the support of the Percutaneous Cardiopulmonary Bypass Support (PCPS), the procedure can be performed very safely, even in patients in ventricular fibrillation. 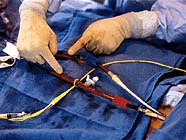 Q:
What kind of impact has PCPS had? Q:
What kind of impact has PCPS had? Dr. Shawl: The use of PCPS has helped many, many patients who otherwise would be crippled and require repeated hospital admissions. Some of them just waiting for a heart transplantation. Many of these patients can now undergo intervention with the PCPS system. On review of the cases and angiographic films, I say, "Listen, you are wait-listed a year or two to receive a new heart; meanwhile let's try this." And of the last dozen cases that I did, over the last two years, four had such improvement that they did not require heart transplantation anymore because of improvement of LV function. The other area where PCPS has played a major role is the sudden cardiac arrest in the cath lab. In these situations it is really a life saver. Q: What alternative do patients have if they cannot undergo bypass or angioplasty? Dr. Shawl: There are many patients who because of small size vessels or diffuse disease are not good candidates for percutaneous interventions or bypass surgery. These patients become severely limited because of incapacitating angina. Percutaneous Transluminal Myocardial Revascularization (PTMR) can provide them with symptomatic relief of angina. In some animals, like crocodiles and alligators, the blood flow to the heart muscle is directly from the LV chamber via small channels. Based on this knowledge, Dr. Mirhoseini created channels in human hearts using laser energy. Over the last few years other surgeons have created similar laser channels directly into the heart muscle with objectively evident beneficial effects. 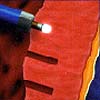 However
the surgical method is more invasive and is associated with 10-19% mortality.
Now, using catheter-based technology, we are able to create channels from
inside the chamber of the heart into the LV muscles. I performed the first
few cases in humans last year in India, without any complications. We are
presently doing PTMR in the U.S. with FDA IDE approval and have done a
number of cases with great success and promising results. I recently presented
the results of these early experiences at the ACC meeting in Atlanta. At
six months 9 out of 12 patients showed objective improvement. However
the surgical method is more invasive and is associated with 10-19% mortality.
Now, using catheter-based technology, we are able to create channels from
inside the chamber of the heart into the LV muscles. I performed the first
few cases in humans last year in India, without any complications. We are
presently doing PTMR in the U.S. with FDA IDE approval and have done a
number of cases with great success and promising results. I recently presented
the results of these early experiences at the ACC meeting in Atlanta. At
six months 9 out of 12 patients showed objective improvement. 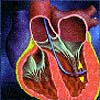 Q:
PTMR is still not approved in the U.S.? Q:
PTMR is still not approved in the U.S.?Dr. Shawl: No, it's still investigational and is being studied in a randomized fashion as per FDA approval. We are already in phase II period of the study and 90 cases have been done. Any patient who is not a candidate for bypass surgery or percutaneous interventions is eligible for this laser revascularization. 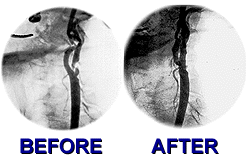 Q:
Can you briefly describe carotid stenting? Q:
Can you briefly describe carotid stenting? Dr. Shawl: Basically it involves the same technique as for coronary angioplasty. Initially we dilate the lesion with balloon angioplasty and then place a stent across the blockage. The whole procedure takes only half an hour to 45 minutes. And the risks are considerably less than carotid surgery even though carotid stenting is just evolving. I am sure that with further refinement in equipment and technique the risk will be even less. Q: I know there is a lot of controversy about carotid stenting. How do you answer these concerns? Dr. Shawl: Well, you know, it is the same as when we started doing coronary angioplasties in the late 70's and early 80's. The concerns were very similar all across the country. Even my surgeons at Walter Reed Army Medical Center, warned me, "Fayaz, don't do it. It is not going to work and the Army will get a bad name." That was then, in 1980. Look at it now, 20 years later, it is the treatment of choice. So it's the same with carotid intervention. Presently there is a lot of skepticism and reservations about this procedure, but having done more than 140 cases in the last two years, I feel it is much safer and far superior to the other methods of treatment which are currently available. I predict that in the next 5 to 6 years this will be the procedure of choice for carotid artery stenosis. We are in the process of arranging a randomized trial. Q: What other areas do you see things moving in? Dr. Shawl: I think an interventional cardiologist will be transformed into what I call a "vascular therapist". He or she will approach every vessel in the human body, from head to toe, particularly in view of the great availability of stents. I also think adjunctive local injection of vascular growth factor shows great promise for many patients who would not be candidates for any form of revascularization. I am also excited about radiation therapy, particularly "beta", which may further reduce the restenosis rate.  Q:
Can you describe the technique of "minimally traumatic angioplasty"? Q:
Can you describe the technique of "minimally traumatic angioplasty"? Dr. Shawl: One of the biggest problems and a persistent thorn in the side of the interventional cardiologist is the phenomenon of 'restenosis'. Richard Myler has shown that the more the trauma to the artery during angioplasty, the more the healing response, and the more the chances for restenosis. In the same context, I think the lesser the trauma, the lesser the healing response and the lesser chance of restenosis. I therefore described a technique of "minimally invasive angioplasty", in which the lowest possible inflation pressure is used to dilate the vessel. If high pressures are needed, first an undersized balloon size is used, followed by a larger balloon. I think that if you can achieve "stent-like" results with balloon angioplasty, then the outcome is no different than stents. And this can be achieved in 30 to 40% of the cases, if balloon angioplasty is performed carefully. So I am not in favor of the prevailing 'stent-mania'. Q: How can a physician tell whether or not to stent? Dr. Shawl: Well, if the vessel is small, for example, less than 2.5mm in size, I would not stent it. In cases of non-ostial right coronary artery or circumflex artery lesions, if the balloon results are good angiographically, than I would not consider stenting it. Q: If the result looks good angiographically, then leave it alone? Dr. Shawl: Yes. Especially in the circumflex and right coronary artery. But if it's a proximal LAD, a vein graft or aorta-ostial, there I would not waste time and I would proceed directly with stenting. I use stents in about 50% of cases, as opposed to others, who use it about 80% of the time. I think you cannot stent every lesion. In cases like bifurcating lesions, long lesions, small vessels, and where there is diffuse disease, stenting actually is associated with higher restenosis rates. Q: So those are not good cases for stenting? Dr. Shawl: Right. In bifurcating lesions, I think rotational atherectomy is far superior and is associated with lesser restenosis. And in diffuse disease I think, along with balloon angioplasty, there is a role for stenting, but stenting only the area which is critical to start with and which does not look good angiographically. This I call "focal stenting". The restenosis with this technique is lower than using a long stent. Q: You wouldn't put like 5 stents in a row.... Dr. Shawl: No, no. That is horrible. They all come back. Q: Do you find that it also compromises future procedures? Dr. Shawl: Oh, absolutely. It makes future interventions very difficult. I am from Gruentzig's school of thought. I believe, "Do what is best for the patient". That is very important to me and I want others to learn likewise. That is the one reason I keep up with the tradition of Andreas Gruentzig, by teaching through demonstration courses both here and abroad. I must admit to you that over the past few years my frustration has been how many interventionalists are very keen to do quickly every form of intervention. I think that is bad. It really takes many many years to develop skill to do what I and others can do. They have to go through the process of learning.  Q:
Your 10th annual course is coming up in May. You show complete cases and
not just the highlights. Why do you show everything, unlike other courses? Q:
Your 10th annual course is coming up in May. You show complete cases and
not just the highlights. Why do you show everything, unlike other courses? Dr. Shawl: I desire to teach from skin to skin. That's my approach. I think people who come to attend the course want to watch everything: the good, the bad and the ugly. I think that's how you learn. I think if you just show them the pre-lesion and the post-lesion, it's just like reading a book or CD-ROM. But live demonstration really means demonstrating the entire procedure. I think it is important to show how to make desirable wire tips, select appropriate balloons, where to park and most important how to avoid complications. Similarly in other situations how to select and deploy a stent and how to easily perform rota-ablation without running into problems. Q: A final question: tell us what is a "hybrid" procedure? Dr. Shawl: I call it the "integrated minimally invasive approach" or "hybrid procedure". You know, I always say, "If bypass surgery were perfect, I would send every patient of mine to surgery." But obviously it's not. The only advantage of conventional bypass surgery is excellent outcome with arterial conduits like LIMA, RIMA, radial or gastroepiploic vessels. We can use these conduits by minimally invasive (MIDCAB) surgery. I see no indication for conventional bypass or use of vein grafts in the 21st century. In patients with multiple vessel disease, instead of conventional CABG, we will use combined MIDCAB and percutaneous intervention. In the last 30 cases or so here at Adventist, we've done MIDCAB first, and then percutaneous interventions to the remaining vessel the next day. And in a few weeks our new operating room / cath lab will be opened, where MIDCAB and percutaneous interventions can be performed at the same sitting. This will be unique and, as far as I know, the first lab to perform bypass and interventions at the same place on the same day. We are very excited about it and hope that it will be a model for the rest of the country and the world. Q: Are you going to be demonstrating a hybrid procedure at your live demonstration course in May? Dr. Shawl: Of course, we will be doing live demonstrations of hybrid cases as well. |
||
This
concludes our interview with Dr. Shawl. In coming weeks,
our series of exclusive interviews with angioplasty pioneers
and leaders will continue with Richard Myler, MD, Patrick
Serruys, MD, Bernhard Meier, MD and many more.  |
||
| |
||
|
Angioplasty.Org Home • PatientCenter send comments & suggestions
to "info at angioplasty dot org" |
||