|
Intravascular Ultrasound
(IVUS) May Reduce Drug-Eluting Stent Thrombosis by a Third
|
 |
July 8, 2008 -- A provocative
study in the current issue of the European
Heart Journal concludes
that:
"IVUS guidance during
DES implantation has the potential to influence treatment strategy
and reduce both
DES
thrombosis and
the need for repeat revascularization."
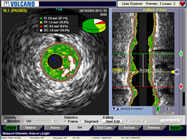
Intravascular
Ultrasound Console
courtesy: Volcano Corporation |
|
The article
describes a retrospective observational study of almost 1,800
patients in whom drug-eluting
stents had been placed between April 2003 and May 2006 at a single
center: the Washington Hospital Center in Washington, DC, where
IVUS guidance is used in approximately
70%
of coronary interventions.
The patient population was split into two groups (IVUS and
non-IVUS) of 884 each, using a propensity-score for matching,
in order to
minimize
any confounding impact due to lesion type, patient characteristics,
etc. |
The clinical endpoint
of the study was definite stent thrombosis at 12 months, which was
measured at three intervals: in-hospital, at 30 days and again at
one year.
The
results were striking, surprising
even the investigators. At 12 months, definite stent thrombosis had
occurred in 0.7% of the patients in whom intravascular ultrasound
guidance had been utilized, but in patients where IVUS was not used,
the
stent thrombosis rate was 2.0%, almost three times higher.
The advantages of IVUS have been written about
extensively, but there has never been a study published that showed
IVUS benefitted patients with drug-eluting stents in terms of stent
thrombosis. Dr. Ron Waksman, corresponding author of the study, told
Angioplasty.Org:
"There are
some situations in which IVUS tells you a lot: for example,
in-stent restenosis.
If you want to know whether this is a mechanical issue versus
a tissue issue, IVUS is very helpful.
If you go to selection of [stent] length and size, that applies to every lesion.
Even if you think that you know the size, you may be surprised
that
you are not accurate just by doing angiography alone.
So there are a lot of helpful hints that you can get from IVUS.
"But perhaps the
most important one applying to the drug-eluting stent is
to obtain sufficient cross-sectional area after deployment
of
the stent -- to see that indeed the stent
is well-expanded, and also well-apposed to the
vessel wall. But I think the emphasis is on expansion, because
sometimes
you can miss on the expansion of the stent without an IVUS.
Again, I think systematic use of IVUS post-stenting, enabling
you to
ensure expansion, to get the ideal cross-sectional area,
probably will you get you out of trouble or may in the future." |
|

Ron Waksman,
MD,
FACC,
Washington Hospital Center
|
If a stent is not fully expanded against the arterial
wall, the small nooks and crannies left between the stent and wall
can be a nexus for platelet aggregation, resulting in a blood clot,
otherwise
known as stent thrombosis -- which can be very serious. Dr. Waksman
explained that most of the stent thrombosis
in the study occurred in the first 30 days, and that this type of
stent thrombosis
is more related to mechanical issues, whereas late stent
thrombosis, occurring after a year or more, is more tied to healing
and inflammation or responsiveness to Plavix. His study only dealt
with the type of stent thrombosis occurring in the first year --
which also occurs more frequently than the late type.
The study also concludes the IVUS guidance "has
the potential to influence treatment strategy" because IVUS can show
information about the lesion in a way that standard angiography cannot:
for example, whether the lesion is eccentric, jagged, calcified in
certain areas -- information that might suggest the use of a cutting
balloon or Rotablator atherectomy device to pre-treat the lesion
and allow the stent to fit more uniformly. In the case of a bifurcation
lesion, Dr. Waksman felt that IVUS would be "almost essential" in
order to judge whether the two stents have been completely expanded.
The results of the study showed no significant
difference in death or MI, but did reveal a trend toward lower target
lesion revascularization (TLR) in the IVUS patients (5.1% as opposed
to 7.2%) suggesting that IVUS use may also impact the occurence of
restenosis.
With IVUS use in the United States hovering in
the low teens, Dr. Waksman feels that more interventional cardiologists
should be thinking about it. He told Angioplasty.Org:
"I would think that 13% is not sufficient,
so there is room to be more liberal with the use of IVUS. The
excuse that
it's cumbersome is fading slowly because we have now integrated
systems, so I think that at this point this is becoming a more
essential tool
and there are really not many complications associated with it.
As to it being time-consuming, it's also becoming relatively
simple
to use.
"So I would encourage cardiologists to
use it more, just based on those results because, now that we've
been
published,
I think
that this is an opportunity for even good operators to end with
better outcomes. And if that's the case, then it's definitely
important
also for those who feel less comfortable in the cath lab with
complex angioplasty. Here we have a tool that can optimize your
result and
you should not spare it on the patient."
Reported by Burt Cohen, July 8, 2008
|



