Angioplasty.Org Interview Series:
Armin Zadeh, MD |
 |
| In this
second in a series of interviews with physicians working in the
field of diagnostic cardiac imaging, Angioplasty.Org talked with
Armin
Zadeh, MD of Johns
Hopkins School of Medicine in Baltimore, Maryland,
where in January Dr. Zadeh will become Director
of Cardiac CT. Dr. Zadeh is currently completing his work on the
ground-breaking CorE 64 study, which will compare current state-of-the-art
64-slice CT angiography with standard invasive angiography done
via cardiac catheterization. The study is due to be presented in
February 2007 and is sure to advance the knowledge of this field
significantly.
Johns Hopkins will also be the first site in the United States
to receive a 256-slice
CT system (from Toshiba America Medical
Systems) for testing.
For an illustrated description of MSCT, read
our related article, Multislice
CT Angiogram. |
|
 Armin Zadeh,
MD
Armin Zadeh,
MD |
|
Q: How accurate is Multislice CT
angiography? Will it replace standard catheterization?
Dr. Zadeh: You have to look at what is available now, what is the evidence supporting
CT now? At this point there are multiple single-center studies suggesting that
the accuracy in detecting what we call obstructive coronary artery disease, usually
defined as at least 50% diameter stenosis, usually associated with ischemia and
symptoms, the detection of this is very high with CT.
There are certain limitations with these
single center studies because they are all performed at very
specialized centers. It's usually not
at an independent core lab. So the question is how can you really generalize
these data to your hospital around the corner? The best way to address this
is to do a multi-center trial. This is currently underway
for the most current generation
64-slice
scanners
and
the results
should
be
available in the next few months. We
do have the results for the 16-slice CT scanners which kind
of indicated that with this generation of scanners,
at least, you would not be able to replace coronary angiography.
|

Johns
Hopkins
Medical Center
in Baltimore, Maryland
|
|
Q: The name of this new trial at Johns Hopkins
is the CorE 64?
Zadeh: Yes. The results will be released real
soon. So how accurate is this technology right now in eliminating
a lot of these cardiac catheterizations? There's clearly
a need to do this because we know from data that at least
30-40% of diagnostic cardiac catheterizations are being performed
with the result of non-significant coronary artery disease.
So there is probably a big chunk of unnecessary invasive
procedures which carry a risk. And the risk of invasive angiography
is often downplayed, but if you look at the data, the complication
statistically at least of dying with a diagnostic cardiac
catheterization is 1 in 1,000. There's still 1 in 500 of
having strokes.
|
Q: One of the
most active
topics in our Patient Forum is complications from
angiograms -- arterial
problems,
nerve
damage, people who have trouble walking. And I think that's
under-appreciated.
Zadeh
: I couldn't agree more. I was just pointing
out the really severe life-threatening complications, but
you're absolutely
right. The vascular complication rate is really quite drastic
and we all know of these cases. We've done hundreds of catheterizations
and we've all experienced them and they are not trivial.
Definitely there is a need, and I think that CT has great
potential just to eliminate these unnecessary invasive procedures.
But again, it's a step process. You have
to look at the data and the multicenter trial will help us
a lot to document
that this is a good tool to diagnose coronary
artery disease. I am convinced that 5 years from now that
we will not do a lot of diagnostic invasive procedures.
It will take a few years just to (A) provide
the data; (B) to convince cardiologists and referring physicians
that this
technology really is ready. But it will happen. Maybe 5 or
6 years from now, but it will be there. And the reason I'm
saying that, I am doing this every day and I see the CT angiograms
and I see the referrals to the cath lab and my personal
experience is also that correlation is very good. Now it
all depends on the quality of the CT angiogram. If you have
a good quality CT angiogram, the information you derive from
the CT angiogram is superior to that of a coronary angiogram
obtained by invasive angiography. And the reason I'm saying
that is because there is evidence from comparisons with intravascular
ultrasound that you do see small changes in the
coronary tree which is not apparent by coronary angiogram.
It's only
seen by intravascular ultrasound. So we're getting information
that we haven't been getting with invasive coronary angiograms.
So it's extremely exciting to detect disease before it becomes
obstructive.
But then that opens a new door and I want
to stick to the discussion: the ability of CT to replace
angiography. So
the quality of the CT angiogram is critical. If you have
a good quality CT angiogram then I think it's at least
as good, and I think it's better than an invasive coronary
angiogram.
The problem is that you don't always get a good quality
CT angiogram at the present time and that's where a lot of
development
is on the way right now.
 Aquilion™ 64-slice
CT scanner** Aquilion™ 64-slice
CT scanner**
|
|
Q: What are the characteristics of a good
quality CT angiogram?
A: In 64 slice CT the main criteria are heart
rate control, patient selection and the absence of heart
rhythm abnormalities. These are the three key factors.
There are differences in detector design but I would say
overall, they're fairly small. More important is that you
have a good heart rate control, meaning that you'd better
look to patients with a heart rate less than 60. And that
you have patient selection. And you have bigger problems
with very obese patients. And lastly if you have atrial
fibrillation that may cause trouble in terms of good image
quality at the time. |
Q: On a different subject,
many times, women present differently than men with heart
problems and chest
pains.
And
often some of the ultrasound and thallium
scan studies have more false positives with female patients.
A: I completely subscribe to that. Definitely
women are more difficult in the sense of diagnosing CAD. We
see a lot
more women who had a thallium stress test where there was
a suggestion of ischemia -- they have more breast intonation
artifacts, particularly in the anterior wall, so they frequently
present
with an abnormal stress thallium and have absolutely normal
arteries by CT angiogram.
The other problem with them
is that they present more with atypical symptoms. And then
they are have abnormal treadmill testing where also women
are known for having more false positive EKG changes. The
EKG changes are often more non-specific and they are harder
to diagnose. You see more women with positive stress
test results who then end up having normal coronary arteries.
At the same time, women also create a problem for CTA in
the sense that they are more sensitive to radiation, and
you have to be more careful, because of the increased risk
for breast cancer. Particularly for younger women it' more
of an issue. And I'm more hesitant, especially with this
generation of scanners, to scan women less than the age
of 40.
Q: Will the more advanced scanners have more or less radiation,
for example the 256-slice scanner? I've read a study that
shows it will have less radiation.
A: The technology is marching
forth at incredible speed. Image quality is getting better
and better, producing more consistently good quality, but
at the same time, radiation is actually going down. There
are several strategies right now to reduce radiation exposure
to the patient and one is using the 256-slice scanner. It
is true that, if you are reducing your scan time, you're
also likely reducing your radiation exposure. We are actually
very interested in exploring this, as soon as we have this
scanner. We are going to get it in just a few weeks. And
that is very exciting to see that we'll be getting better
image quality at lower radiation exposure.
We are actually
expecting to have quite drastic reductions because we also
are doing all retrospective gating, meaning we are acquiring
images throughout the cardiac cycle, whereas a lot of recent
developments have shown that you may be able to obtain
good quality images while you just obtaining images during
a specific
part of the cardiac cycle. Meaning that the radiation exposure
will be further reduced to a very short fraction, well
within the cardiac cycle. So there are several developments
ongoing
that are very promising. What we see right now
is the peak of the radiation exposure and it will only
get better and some studies are suggestions that it will
get
a lot better, meaning that radiation exposure will be cut
by 60, 70 or even 80%.
The reason for that is the improvement in detector design,
more coverage, prospective gating. The dual source CT apparently
has shown quite a reduction in radiation dose. There are
several strategies that we need to pursue and it is very
exciting to see how it will all pan out in the next few months
and years.
Q: There's some confusion out there about CT
scans. Can you explain the difference between a Multislice
CT angiogram and a CT calcium scoring test? And do you
think calcium scoring exams, with no contrast, are useful?
A: They are useful because they provide us
with prognostic data. Now we're going into the whole area
of primary prevention, where we're trying to establish in
asymptomatic people what is the risk of having obstructive
or meaningful coronary artery disease.
Our current ways to assess this are extremely limited: we
have the Framingham risk score, which has shown over and
over and over that it works well in overall populations,
but for risk protection in a given individual, it's extremely
limited. |
The
Calcium score has ten years plus of data showing that it IS
predictive. Higher Calcium scores are predictive of obstructive
coronary
disease and of coronary events. And vice-versa, if you have
no Calcium in your coronaries, then you have very low risk
of having
events and obstructive disease.
So I do Calcium scores on almost
everybody because there's no contrast involved, the radiation
dose is very, very low, and you do get information and prognostic
data.
And I continue
to be amazed that the current guidelines still haven't
adopted this. There's talk about including CRP, but calcium
scoring
has much more compelling data. Nevertheless, it hasn't
been incorporated into the overall risk model. The SHAPE
guidelines were
very interesting and very provocative. I think calcium scoring
has a lot of merit
and it comes with low toxicity and cost. And you can do
it
at very low settings, like 1.5-2 millisieverts which
is less than
the average annual exposure of the American adult. |
|
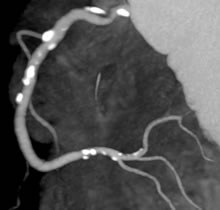 A
Calcium plaque score done on a multislice CT scanner,
using 3D Maximum Intensity Projection (MIP) of CT
A
Calcium plaque score done on a multislice CT scanner,
using 3D Maximum Intensity Projection (MIP) of CT |
Q: There was
a recent article in the NYT about vulnerable plaque and
it talked a
lot about CT as a way of visualizing vulnerable plaque.
I've been told that this is not yet "ready for
prime time".
A: We don't know. It's too early in the game.
We do see a lot of things, we do see plaque, for instance,
in the proximal LAD or left main which would be a "poster
child" for what vulnerable plaque looks like. Or then we
have a large non-calcified plaque burden with low-density
content
which you could think could be a lipid core, etc. So I
have seen those, but we have no clues that
these are really vulnerable, and you need a lot of data
and pathology and intravascular ultrasound data, and long-term
follow-up to know exactly what constitutes vulnerability
by CT.
Having said all that, some people like
Peter Libby doubt that there
is such a thing as a vulnerable plaque. If you look at
the
pathology data, I spoke with Renu Virmani, first of all,
only 50-60% of plaques done by pathology which we think
were causing MI had these characteristics of the lipid
core. There are a lot of other plaques which have fissures,
a lot of other plaques which have none of these characteristics
and which turn out to be the culprit lesions. It's not
that straight-forward.
And there's data that turned up in another
one of Dr. Virmani's publications that looked at patients
who died of a non-cardiac death, clearly non-cardiac death,
an accident or whatever. They found 10% of those had evidence
of prior plaque rupture. So that tells me that plaque rupture
is much more common than we think it is, but only in a
minority of cases actually leads to a devastating event.
It means even if we find plaques that are possibly at risk,
it still doesn’t mean that they'll cause you a lot
of harm. This data suggests that this is much more complex,
this picture. It only leads to a catastrophic event if
some other factors are involved as well: for example the
whole coagulation and platelet function issues. This is
a very complex issue and sometimes we try to make it too
easy and say, you know, we have to chase after vulnerable
plaque and you're going to solve the issue.
Q: What else is on the horizon
for CT?
A: The other thing which is not well-publicized
right now is the potential for CT also to do perfusion
imaging. It's something we're very excited about. We're
currently conducting a clinical trial here where we are
looking at stress perfusion with CT. This would not be
a higher dose than is currently seen with Thallium scans,
hopefully a lower dose, and with much better resolution.
And again, you're getting both: you're getting the coronaries
AND at the same time, you're getting artery perfusion.
This is extremely interesting. Why would you get a nuclear
perfusion study when you could get it all with CT? Because
if you look at the meta-analysis of nuclear stress perfusion,
it's not that great. The sensitivity is something like
80-82%. And the specificity is 76%.
We've given millions of nuclear stress
tests to people and never even thought about these things,
and now radiation is a big issue, and rightly so, but it
should have been a big issue ten years ago when all these
nuclear stress tests were done. So the 256 actually will
be very interesting for the whole stress perfusion research.
Eventually I think there's not
going to be much need for nuclear scans, if it pans out
the way I think it will, that you can do these tests
with CT better.
|
|
| This interview was conducted in November
2006 by Burt Cohen of Angioplasty.Org. |
| ** photo courtesy of
Toshiba America Medical Systems |
|
|
