Angioplasty.Org Interview Series:
Daniel Berman, MD, FACC |
 |
| Daniel S. Berman,
MD, FACC, is a Professor of Medicine at the UCLA School of Medicine
and Director of Cardiac Imaging at Cedars-Sinai
Medical
Center in Los Angeles, where he has led the invasive group for 29
years. Dr. Berman is also the Vice-President of the Society
of Cardiovascular
Computed Tomography, which just celebrated its first
anniversary.
The rapid
development of Multislice Computed Tomography (MSCT) is changing
the way patients with suspected coronary artery disease are being
diagnosed. Until just a few years ago, standard coronary angiography
(cardiac catheterization) was the only way to visualize the coronary
arteries. By comparison, MSCT is faster, less expensive and less
invasive.
For an illustrated description of MSCT, read our related article, Multislice CT Angiogram.
|
 Daniel S. Berman,
MD,
FACC
Daniel S. Berman,
MD,
FACC |
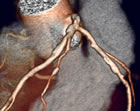 "Multislice
CT angiography is...undoubtedly the most accurate non-invasive
test for the diagnosis of obstructive
coronary disease" **
"Multislice
CT angiography is...undoubtedly the most accurate non-invasive
test for the diagnosis of obstructive
coronary disease" ** |
|
Q:
How is the availability of 64-slice or Multislice CT
for patients changing the
diagnostic pathway from what is used to be?
Dr. Berman: What’s happening with Multislice CT is that it is going to
change the way we approach the patient with chest pain in terms of establishing
the cause.
The main area where the impact will
be felt initially is in chest pain that isn’t characteristic of being from heart disease, but could be.
We call this the intermediate likelihood state of having coronary artery disease.
And it’s been known for years that that’s the time in which you use
the most accurate test that’s non-invasive to establish the diagnosis.
That’s what Multislice CT angiography is. It’s undoubtedly the
most accurate non-invasive test for the diagnosis of obstructive coronary disease. |
Q: Exactly who
is the patient with intermediate risk?
Dr. Berman: Every doctor who sees a patient
that could be cardiac is thinking in his mind, what’s
the likelihood that this patient’s symptoms are related
to coronary artery disease?
Clinicians define coronary disease as a greater than 50%
stenosis of a coronary vessel. Some people use 50%, some
people use 70%. But when they talk about coronary artery
disease, clinicians do not mean just the presence of coronary
atherosclerosis. It’s not just plaque; it’s obstructive plaque
causing chest pain. |
|
|
| When patients have typical angina pectoris,
it comes on with exertion, is relieved by rest, and is in
the middle of the chest. If they’re in the appropriate
age group, the chances of them having coronary disease are
about 90%. That’s a high likelihood of having coronary
disease. Experts in general, do not believe that’s
the group that needs Multislice CT scan.
But if you take a patient whose chest discomfort symptoms
are less typical, the likelihood that they have obstructive
coronary disease falls in the [intermediate]
range between 25 to 75% likely that a patient’s symptoms
might be explained on the basis of obstructive coronary
disease.
These are decisions that a doctor, whether it’s
a family practitioner, an internist or a cardiologist make
when they are faced with a patient who has chest discomfort
or shortness of breath symptoms that might be attributed
to the heart. In the intermediate likelihood range, we
use the test with the highest sensitivity and specificity
for detecting
obstructive disease -- and that test is the CT coronary
angiogram. |
Q:
WIll 64-slice CT replace coronary angiography as a diagnostic
modality -- or, as some physicians feel, will the impact
be more on other diagnostic tests like thallium scans
and echo stress tests?
Dr. Berman: The diagnostic coronary angiogram
isn’t really a very common test anymore. I’ll
bet if we were to survey the number of coronary angiographies
done in the United States today that are done just for the
purposes of establishing a diagnosis, with no intention of
doing angioplasty, it would be a very small number.
The area
that will be most affected will be the area in which tests
have been used traditionally
in patients with an intermediate likelihood of having coronary
disease. And that isn’t the diagnostic coronary angiogram;
that’s stress imaging, whether it’s a stress
nuclear procedure or a stress echo procedure, or even a stress
test. I think those tests may actually decline in their use
for diagnosis of coronary disease. |
|
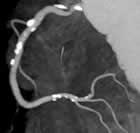 3D
Maximum Intensity Projection (MIP) of CT, showing calcified
plaque**
3D
Maximum Intensity Projection (MIP) of CT, showing calcified
plaque** |
| But when you look at the big picture of the use of tests,
those other tests may increase in another population. In
the people who have already known coronary disease. And,
as the baby boomers age, there’ll be more and more
in that age group. So it’s complex.
There
still will be diagnostic applications. There still will
be a lot of use of nuclear testing. But
the first test of choice in the patient with intermediate
likelihood of coronary artery disease who has symptoms may
well become the CT coronary angiogram.
Q: What is the impact on and
the experience of the patient during multislice CT scanning?
Dr. Berman: It’s a very rapid test that
involves about 15 minutes of time, and an injection of a contrast
agent that does cause a warm sensation. There is a small risk
of an allergic reaction to this injected contrast and, in that
sense, it differs from other methods such as MRI or nuclear
cardiology technologies that also use injections but without
that risk of allergy.
The other thing that can happen is that
there’s a small risk of kidney impairment on the basis
of giving this dye, so patients who have kidney dysfunction
or abnormally functioning kidneys are approached very cautiously.
There are ways around these risks, however,
and they are very small.
There is a radiation exposure associated
with the test, but it’s similar to the radiation exposure
of other diagnostic tests. Because of the radiation exposure
we are not currently recommending that this be used as a
screening test for everyone. We would want to use a test
with less radiation unless there was a higher suspicion of
obstructive
disease. But in the future, that radiation burden may
be decreasing significantly.
Q: How do you see the future
developments in Multislice CT in terms of the ability
to use less radiation, and other advances?
Dr. Berman: In the near future, techniques to
reduce the radiation exposure will be developed. There will
be increased ability to objectively analyze the images so that
we don’t rely just on the skill of the operator of the
computer workstation And there will be improvement in technology
that may reduce the need to rely on beta-blockers to slow the
heart rate sufficiently in all cases.
Q: Which professional should
be doing Multislice CT scanning for coronary artery disease
-- the cardiologist, radiologist, etc.?
Dr. Berman: It’s going to be done by
whoever is the best trained in a given circumstance. They
will range from people who are doing catheterizations now,
to people whose specialty is noninvasive imaging to people
whose specialty is radiology with a focus on cardiovascular
imaging. I don’t think it’s so much what the
person’s area of general specialization is as much
as it is what is the person’s skill and expertise in
this specific form of testing.
Q: What about Magnetic Resonance
Angiography (MRA)?
Dr. Berman: Not going to be a player for the
coronary artery because of limitations in multiple different
problems that arise for looking at coronary arteries. MRA will
be helpful in assessing plaque in other vessels, but coronary
artery disease that is such a prominent killer can be active
at a time when disease is not active in other vessels in the
system, so it’s not as direct an approach as will be
provided by plaque imaging using the coronary artery and PET/CT.
Q: In recent years, it's become
clear that it's not just the amount of plaque, but the
type of plaque that is important to visualize. What is
the status of Multislice CT scanning right now with the
imaging of different forms of plaque?
Dr. Berman: It’s completely in the research
phase and I think it’s premature to say how that’s
going to affect patient management. Right now, the amount of
soft, of non-calcified, plaque that a patient has -- it shouldn’t
be called soft, because often it’s hard, but it’s non-calcified plaque
-- can be evaluated in CT in a way that can’t be achieved
by any other current technique in the coronary artery. Even
the diagnostic coronary angiogram can’t see the non-calcified
plaque -- it sees the lumen rather than the wall of the vessel.
We believe that in the more distant future,
we will have techniques that will allow us to assess, to
identify patients with rupture-prone plaque, which is probably
a better term than vulnerable plaque. The rupture-prone plaque
is a plaque that is associated with inflammation, a lot of
lipid disposition, and has a thin cap on the plaque. The
features of inflammation may give us a specific target that
could be used in combination with PET scanning and CT scanning
in the future.
So looking down the line, I believe that
instead of just simply saying that we’ll find patients
who have coronary obstruction, we’re going to ultimately
have the ability to separate out the people who are at very
high risk by identifying patients who have rupture-prone
plaque. I also believe that it’s going to be difficult
to do that with CT alone and it may require a technique such
PET/CT. |
Q: You currently are Vice-President
of the Society of Cardiovascular Computed Tomography (SCCT).
Tell me about the organization, especially with regard
to training.
Dr. Berman: Well the Society of Cardiovascular
Computed Tomography is really set up to do whatever is necessary
to help new technology reach its true potential. And that’s
a broad statement, but that’s what all of us as the founders
really feel is the mission. The mission statement is on the web
site, and it’s really been carefully thought
out. I think in simple terms -- it’s to do what is necessary
to allow this promising new technique to reach its full potential
in patient care. |
|
|
|
 "Multislice
CT angiography is...undoubtedly the most accurate non-invasive
test for the diagnosis of obstructive
coronary disease" **
"Multislice
CT angiography is...undoubtedly the most accurate non-invasive
test for the diagnosis of obstructive
coronary disease" ** |
|
Q:
How is the availability of 64-slice or Multislice CT
for patients changing the
diagnostic pathway from what is used to be?
Dr. Berman: What’s happening with Multislice CT is that it is going to
change the way we approach the patient with chest pain in terms of establishing
the cause.
The main area where the impact will
be felt initially is in chest pain that isn’t characteristic of being from heart disease, but could be.
We call this the intermediate likelihood state of having coronary artery disease.
And it’s been known for years that that’s the time in which you use
the most accurate test that’s non-invasive to establish the diagnosis.
That’s what Multislice CT angiography is. It’s undoubtedly the
most accurate non-invasive test for the diagnosis of obstructive coronary disease. |
Q: Exactly who
is the patient with intermediate risk?
Dr. Berman: Every doctor who sees a patient
that could be cardiac is thinking in his mind, what’s
the likelihood that this patient’s symptoms are related
to coronary artery disease?
Clinicians define coronary disease as a greater than 50%
stenosis of a coronary vessel. Some people use 50%, some
people use 70%. But when they talk about coronary artery
disease, clinicians do not mean just the presence of coronary
atherosclerosis. It’s not just plaque; it’s obstructive plaque
causing chest pain. | |
|
| When patients have typical angina pectoris,
it comes on with exertion, is relieved by rest, and is in
the middle of the chest. If they’re in the appropriate
age group, the chances of them having coronary disease are
about 90%. That’s a high likelihood of having coronary
disease. Experts in general, do not believe that’s
the group that needs Multislice CT scan.
But if you take a patient whose chest discomfort symptoms
are less typical, the likelihood that they have obstructive
coronary disease falls in the [intermediate]
range between 25 to 75% likely that a patient’s symptoms
might be explained on the basis of obstructive coronary
disease.
These are decisions that a doctor, whether it’s
a family practitioner, an internist or a cardiologist make
when they are faced with a patient who has chest discomfort
or shortness of breath symptoms that might be attributed
to the heart. In the intermediate likelihood range, we
use the test with the highest sensitivity and specificity
for detecting
obstructive disease -- and that test is the CT coronary
angiogram. |
Q:
WIll 64-slice CT replace coronary angiography as a diagnostic
modality -- or, as some physicians feel, will the impact
be more on other diagnostic tests like thallium scans
and echo stress tests?
Dr. Berman: The diagnostic coronary angiogram
isn’t really a very common test anymore. I’ll
bet if we were to survey the number of coronary angiographies
done in the United States today that are done just for the
purposes of establishing a diagnosis, with no intention of
doing angioplasty, it would be a very small number.
The area
that will be most affected will be the area in which tests
have been used traditionally
in patients with an intermediate likelihood of having coronary
disease. And that isn’t the diagnostic coronary angiogram;
that’s stress imaging, whether it’s a stress
nuclear procedure or a stress echo procedure, or even a stress
test. I think those tests may actually decline in their use
for diagnosis of coronary disease. | |
 3D
Maximum Intensity Projection (MIP) of CT, showing calcified
plaque**
3D
Maximum Intensity Projection (MIP) of CT, showing calcified
plaque** |
| But when you look at the big picture of the use of tests,
those other tests may increase in another population. In
the people who have already known coronary disease. And,
as the baby boomers age, there’ll be more and more
in that age group. So it’s complex.
There
still will be diagnostic applications. There still will
be a lot of use of nuclear testing. But
the first test of choice in the patient with intermediate
likelihood of coronary artery disease who has symptoms may
well become the CT coronary angiogram.
Q: What is the impact on and
the experience of the patient during multislice CT scanning?
Dr. Berman: It’s a very rapid test that
involves about 15 minutes of time, and an injection of a contrast
agent that does cause a warm sensation. There is a small risk
of an allergic reaction to this injected contrast and, in that
sense, it differs from other methods such as MRI or nuclear
cardiology technologies that also use injections but without
that risk of allergy.
The other thing that can happen is that
there’s a small risk of kidney impairment on the basis
of giving this dye, so patients who have kidney dysfunction
or abnormally functioning kidneys are approached very cautiously.
There are ways around these risks, however,
and they are very small.
There is a radiation exposure associated
with the test, but it’s similar to the radiation exposure
of other diagnostic tests. Because of the radiation exposure
we are not currently recommending that this be used as a
screening test for everyone. We would want to use a test
with less radiation unless there was a higher suspicion of
obstructive
disease. But in the future, that radiation burden may
be decreasing significantly.
Q: How do you see the future
developments in Multislice CT in terms of the ability
to use less radiation, and other advances?
Dr. Berman: In the near future, techniques to
reduce the radiation exposure will be developed. There will
be increased ability to objectively analyze the images so that
we don’t rely just on the skill of the operator of the
computer workstation And there will be improvement in technology
that may reduce the need to rely on beta-blockers to slow the
heart rate sufficiently in all cases.
Q: Which professional should
be doing Multislice CT scanning for coronary artery disease
-- the cardiologist, radiologist, etc.?
Dr. Berman: It’s going to be done by
whoever is the best trained in a given circumstance. They
will range from people who are doing catheterizations now,
to people whose specialty is noninvasive imaging to people
whose specialty is radiology with a focus on cardiovascular
imaging. I don’t think it’s so much what the
person’s area of general specialization is as much
as it is what is the person’s skill and expertise in
this specific form of testing.
Q: What about Magnetic Resonance
Angiography (MRA)?
Dr. Berman: Not going to be a player for the
coronary artery because of limitations in multiple different
problems that arise for looking at coronary arteries. MRA will
be helpful in assessing plaque in other vessels, but coronary
artery disease that is such a prominent killer can be active
at a time when disease is not active in other vessels in the
system, so it’s not as direct an approach as will be
provided by plaque imaging using the coronary artery and PET/CT.
Q: In recent years, it's become
clear that it's not just the amount of plaque, but the
type of plaque that is important to visualize. What is
the status of Multislice CT scanning right now with the
imaging of different forms of plaque?
Dr. Berman: It’s completely in the research
phase and I think it’s premature to say how that’s
going to affect patient management. Right now, the amount of
soft, of non-calcified, plaque that a patient has -- it shouldn’t
be called soft, because often it’s hard, but it’s non-calcified plaque
-- can be evaluated in CT in a way that can’t be achieved
by any other current technique in the coronary artery. Even
the diagnostic coronary angiogram can’t see the non-calcified
plaque -- it sees the lumen rather than the wall of the vessel.
We believe that in the more distant future,
we will have techniques that will allow us to assess, to
identify patients with rupture-prone plaque, which is probably
a better term than vulnerable plaque. The rupture-prone plaque
is a plaque that is associated with inflammation, a lot of
lipid disposition, and has a thin cap on the plaque. The
features of inflammation may give us a specific target that
could be used in combination with PET scanning and CT scanning
in the future.
So looking down the line, I believe that
instead of just simply saying that we’ll find patients
who have coronary obstruction, we’re going to ultimately
have the ability to separate out the people who are at very
high risk by identifying patients who have rupture-prone
plaque. I also believe that it’s going to be difficult
to do that with CT alone and it may require a technique such
PET/CT. |
Q: You currently are Vice-President
of the Society of Cardiovascular Computed Tomography (SCCT).
Tell me about the organization, especially with regard
to training.
Dr. Berman: Well the Society of Cardiovascular
Computed Tomography is really set up to do whatever is necessary
to help new technology reach its true potential. And that’s
a broad statement, but that’s what all of us as the founders
really feel is the mission. The mission statement is on the web
site, and it’s really been carefully thought
out. I think in simple terms -- it’s to do what is necessary
to allow this promising new technique to reach its full potential
in patient care. |
|
|
|
This interview was conducted in June
2006 by Burt Cohen of Angioplasty.Org. |
|
|
