 |
 |
 |
Harvey S. Hecht,
MD, FACC, is an internationally recognized expert in cardiac
imaging and preventive cardiology, and is the author of more
than 100 publications in peer reviewed journals. After achieving
acclaim as a leader in the fields of nuclear cardiology and
stress echocardiography, Dr. Hecht pioneered the development
of noninvasive coronary computed tomographic angiography (CTA)
and is a driving force behind CTA guided percutaneous coronary
intervention and the relationship between CTA and intravascular
ultrasound (IVUS). He was the first to demonstrate the poor
relationship between risk factors and atherosclerosis.
Prior to his current position as Director of Cardiovascular
Computed Tomography at Lenox
Hill Heart and Vascular Institute of New York, Dr. Hecht
held numerous faculty, clinical and administrative positions
at institutions ranging from UCLA, USC, UCSF and Albert Einstein
College of Medicine to the San Francisco Heart Institute, Arizona
Heart Institute, Princeton Longevity Center, and Beth Israel
Medical Center. Dr. Hecht is a Fellow of the American College
of Cardiology and member of numerous professional societies,
as well as a founding member of the SCCT. |
|
 Harvey
S. Hecht, MD, FACC
Harvey
S. Hecht, MD, FACC
Lenox Hill Heart and Vascular Institute of New York
|
Q: Given the change in the paradigm
youve
discussed, what then do you see as the role of nuclear stress testing?
Dr. Hecht: Nuclear would be used in the intermediate stenoses, in the 50 to 75% stenosis range to see if there's functional abnormality. If there is, then fine, that lesion is capable of producing ischemia and intervention may be warranted. If the nuclear is normal then presumably the lesion is not capable of producing ischemia.
But, this assumes that nuclear is accurate in that situation, and we know that while the sensitivity of nuclear is pretty good, in the 85% range, there are situations which I've mentioned before, left main disease in particular, in which it's wrong 15% of the time. You can't afford to be wrong in left main disease. Or perhaps it underestimates the second and third vessel stenosis ischemia, because you're comparing one wall to another wall. In general, the use of nuclear stress testing is going to decline. And instead of being the first line, the first test for evaluation, it will follow CTA rather than precede it.
Q: What about the use of CTA in emergency situations? I know there are some studies going on right now, I think William Beaumont in Michigan is doing one?
Dr. Hecht: Yes. This is a superb use, and there are several papers that are published on this already, and again, it's a paradigm shift. Rather than get serial sets of enzymes and EKGs and then send the patient for a nuclear test or a stress echo, as soon as the first EKG and enzyme have been obtained and the patient is stable and there's no evidence of an infarction, a CTA can be done. If they're having an acute MI or unstable angina, they go straight to the cath lab -- CTA is not appropriate.
So they have the CTA done, and what they have found is this: (1) the time to diagnosis is dramatically decreased from about 14 hours to 4 hours; (2) it's less expensive to do the CTA route, and (3) the need for follow-up evaluation in those patients who are sent home with a normal CTA is less than if they're sent home after a normal nuclear test.
Moreover, in the Emergency Department experience, CTA identifies a cardiac cause about 40% of the time as the explanation for the chest pain visit -- why they came to the emergency room. But what about the other 60%, why did they come there? If you do a nuclear test or a stress echo, you get zero information about any non-cardiac cause for the chest pain, which is the predominant reason for their being in the ED. But when you do a CTA, you get a CT of the chest and so you can find pulmonary causes, you can find GI causes, reflux, you find infiltrates, atelectasis. You can find non-ischemic causes for their complaints, so the patients leave with a diagnosis.
Q: Can a CTA help the interventional cardiologist in the cath lab, in terms of which angle has the best view of the blockage, since you get a 3-dimensional manipulatable model?
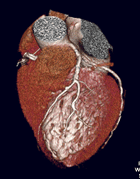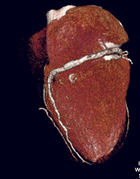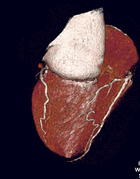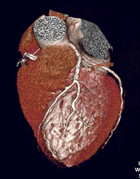
Multislice
CT of the Heart, courtesy of Toshiba America Medical Systems |
|
Dr. Hecht: Well, it facilitates
many areas in the cath lab. By virtue of being able to rotate
the arteries 360 degrees, you can more easily detect a stenosis
that you might have missed with the limited 6 or 7 acquisitions
of the left coronary, maybe 3 of the right coronary artery, that
you typically do in a cath. You have infinite sampling ability
as opposed to the limited sampling that's inherent in the cath
lab.
You also, as we talked about, can readily identify diffuse
segmental narrowing, which will be angiographically inapparent
because there is no normal reference point. CTA can identify
areas of positive and negative remodeling, and in the cath lab
that's very hard to do. So the reference point that's used for
measurement of lesions in the cath lab is, almost invariably,
an area that has positive remodeling, adjacent to the severe
stenosis, so again the degree of stenosis may be overestimated
in the cath lab because you're using really an inaccurate reference
point. |
CTA also gives you information about the nature
of the plaque. You can identify vulnerable plaques, you can identify
the lipid-laden plaques. Currently there's no indication to do anything
interventional, other than medical therapy, for a non-obstructive vulnerable plaque.
That may change once the results of the PROSPECT study are published.
But still, you have the ability to identify that kind of vulnerable
plaque. You also can identify plaque rupture.
You can greatly facilitate opening chronic total occlusions (CTO) because, while in the cath lab the occluded segment may be totally invisible on angiography. But the CTA is always visible. You can always track and identify the occluded segment, and you can draw up a road map for the interventionalist. So, CTA should be an intrinsic part of every CTO attempt. You can also, by rotating the CTA, identify the angiographic view that displays the stenosis in its least foreshortened length. And that view can be reproduced in the cath lab, so you can do more appropriate stent sizing by seeing the lesion in its least foreshortened length.
In addition, you can use CTA itself for stent sizing, both longitudinally because you can more accurately determine what area you want to cover with a stent -- you may decide to cover areas that are not angiographically apparent but on the CTA are obviously quite diseased. And you can do better axial sizing as well, because it's very easy to measure the size of the proximal and distill reference segment.
Q: And, as weve discussed with
intravascular ultrasound, if you underestimate the area when you're
placing a stent,
you're probably opening yourself up to a higher percentage of problems
like restenosis, thrombosis, etc.?
Dr. Hecht: Correct. Exactly. In addition to which, there are certain
situations which you can only address with CTA after the cath has been
done. First of all, in even the most experienced angiographer's hands,
there are the occasions when you cannot cannulate a vessel. Particularly
a graft, a bypass graft. Most often, a right internal mammary or a
vein graft that you just can't find using angiography, but you think
is there. Well, CTA will never miss that. There are also situations
in which, upon introduction of the catheter tip into the ostium of
the left main or the right, you get severe damping, and it would be
dangerous to inject. Are you dealing with spasm, or are you dealing
with tight left main or ostial RCA disease? Again you can answer that
situation very easily by doing a CTA afterwards. The course of anomalous
coronary arteries may be very hard to determine in the cath lab. The
course of bypass grafts is critically important in a re-do operation
for a surgeon to know, Where is that RIMA or that LIMA? Is it right
below the sternum, is he likely to transect it if he goes through the
sternum? That information is very easily provided, in this case, for
the surgeon.
Q: What about CTA as a way of checking
if a stent is still open? We have patients on our Forum who are having
chest
pain and wondering Is my stent closing up? Should they have a CTA?
Dr. Hecht: Here's my take on it. CTA is very, very sensitive. It'll pick up about 90 to 95% of in-stent restenosis. The problem is that the incidence of in-stent restenosis in the drug-eluting stent era is so low, it's in the 12 to 15% range, that the likelihood of a CTA giving you a true positive diagnosis is not that great. This is a perfect application of Bayes' theorem, which says that the accuracy of any test depends upon the prevalence of the disease in the population. If there's a very low likelihood of restenosis because of drug-eluting stents, then the prevalence of that disease is very low. So in a test that's not 100% specific, and no test is, the chance that a positive will be a true positive is probably in the 50% range.
The key is to do the CTA in patients who are symptomatic within the expected time range for restenosis after implantation: six months. Then you're going to have a much higher chance of a positive being a true positive. If you do it in an asymptomatic patient who's had stents in place for two to three years, that's not a situation that I would do the CTA on to look for in-stent restenosis. But for the patient who has recurrent symptoms, I think it's a very appropriate test, especially within the six month period.
Q: Everyone has said this is not a screening tool for asymptomatic patients, but a lot of patients are saying I have family history, I've got high cholesterol, I don't have chest pains, but I'd really rest easier knowing that I don't have this disease.
What would you say to those patients, who want to be screened?
Dr. Hecht: I think, for the vast majority of totally asymptomatic patients who want to be screened, the calcium score alone is the ideal test. The patients for whom it's not adequate are those who have a family history for premature coronary disease, and those patients have an increased risk for events, significantly increased risk. So you want to catch these patients as early as you can -- they will often have a zero calcium score. In that population, doing a CTA to look for significant amounts of non-calcified plaque will better help you risk stratify. And there are a number of us who believe that it is appropriate to use as a screening test in those patients who have a striking family history for premature coronary disease in whom the calcium score would be zero, particularly if we can decrease the radiation dose, which we can.
Q: Its interesting that you advocate
so strongly for CTA. You have a long history with nuclear testing and
nuclear cardiology
prior to the invention of multislice CTA.
Dr. Hecht: Right, I have a huge background in both nuclear and stress echocardiography, and CTA is simply a better test. It's time to move to the better test.
(Return
to Part One)
| This interview was conducted in March
2008 by Burt Cohen of Angioplasty.Org. |
|



