Angioplasty.Org Interview Series:
James K. Min, MD, FACC
|
 |
| James K. Min,
MD, FACC, is Director of Cardiac CT labs
at Weill-Cornell Medical College,
New York-Presbyterian Hospital, and specializes in the diagnosis of coronary heart
disease with multidetector CT angiography. He also has expertise
in echocardiography, nuclear cardiology and the identification
of novel clinical risk factors that place individuals at higher
risk
for the
development
of
coronary
heart disease.
Dr. Min is a member of the Board of Directors of the Society
for Cardiovascular Computed Tomography (SCCT). He received
his medical degree from Temple University School of Medicine
and completed his internship, residency, and cardiology
fellowship at the University of Chicago Hospitals. Dr. Min
is Assistant
Professor of Medicine, Division of Cardiology and Assistant
Professor of Radiology at the Weill Cornell Medical College
and the New York Presbyterian Hospitals in New York City.
He lectures both nationally and internationally on cardiac
CT, has conducted the CT Cardiac Masters
Series for the GE Healthcare Institute and has appeared
on national television to discuss the impact of cardiac CT
on
clinical
cardiology
practice.
He
is co-author of the Cardiac CT Atlas. |
|
 James
K. Min, MD, FACC
James
K. Min, MD, FACC
NewYork-Presbyterian Hospital |
Q: Where would you place coronary
CT angiography right now in the spectrum of diagnostic tests
for coronary artery disease? Is it a first line
test? Or should other tests be done before it?
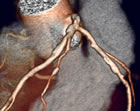
64 slice
CT Angiogram
of coronary artery |
|
Dr. Min: That's a good question.
I think its greatest role is in symptomatic patients of low intermediate
to intermediate risk. Patients without known coronary disease
who present with certain chest symptoms can be first evaluated
very effectively with coronary CT angiography (CCTA).
I think
its greatest use at the present time -- I think it will change,
it's a work in progress -- but I think that its greatest use
today is in the exclusion of significant coronary disease in
patients who don't have any and they then don't need any further
testing. |
Q: What are the implications of that for patients?
Dr. Min: When patients come to my office and complain of chest pain,
they want to know whether they have coronary disease or not. And
they want to know whether or not they have severe enough coronary
disease that treatment mandates medical therapy or more invasive
therapy. Ultimately they want to know how they're going to do,
based on that treatment.
The historical tests that we have identify coronary atherosclerosis
at a much later stage. Oftentimes the normal functional stress tests
are not able to say that somebody is free of coronary artery disease,
so to be able to give a person either an exclusion or a diagnosis
of coronary artery disease (CAD) is the first step in the process.
The second question is what to do with the finding
of that test. If you have non-obstructive mild CAD in a symptomatic
patient with
other risk factors, then medical treatment is probably warranted.
In the patient with obstructive CAD, that's going to be at the discretion
of who is treating that person. An argument could be made that direct
referral to angiography with percutaneous intervention of an obstructive
lesion for symptom benefit is beneficial, or one could argue that
were it not surgical disease (i.e. left main, three vessel or proximal
LAD disease) that initial medical management could be warranted with
downstream cross-over if symptoms couldn't be controlled with medical
therapy.
Q: One of the criticisms is that there is an overuse of CCTA.
Dr. Min: I don't think it is overused. If you compare its use to
that of the nuclear imaging stress test, it pales in comparison.
So it is not yet over-used. Does it have the potential to be overused?
I suppose anything has the potential to be overused. I think the
goal is to try to find appropriate indications for its use in clinical
practice that benefits patients. I think that appropriateness criteria
have gone a far way to help delineate for which indications CCTA
may be most useful. I think that the soon-to-be-released consensus
guidelines on coronary CT angiograms are going to help. I think
that the awareness in the field is that diagnostic tests should
achieve a certain sense of clinical and cost efficiency. That's
an admirable goal. In that vein, I think that governing bodies,
the ACC in particular, have championed this idea of appropriateness,
as it relates to the implementation and efficiency.
Q: Patients write into our Forum that they are being sent to have
an invasive catheterization because of an abnormal stress test. Is
this a typical scenario?
Dr. Min: It's not an infrequent clinical scenario. Probably as a
result of being a tertiary referral lab, we see a fair number of
patients after nuclear stress testing and we can sort of debate where
CT should fit: should it fit before, as a first line test, or after,
as an arbiter to nuclear stress testing? We see not a trivial amount
of patients, who come to us after having an abnormal stress test.
CT is good at arbitrating those abnormalities. If there are artifacts
or if it’s an equivocal stress test or it's a normal stress
test with persistent symptoms, CT is pretty good at arbitrating those.
Q: NCDR data shows that over
1/3 of invasive angiograms done in the cath lab show no significant
disease. Could those patients have avoided the cath lab if they
had gotten a CT angiogram instead?
Dr. Min: Probably. Because
we know that CT's negative predictive value approaches 100% --
so you literally exclude significant coronary artery disease
with a 99% certainty. There was a study that looked at that out
of Chicago, where they took patients with moderately abnormal
stress tests and used CT to arbiter that. And if that person
had severe coronary disease in the area of interest of the nuclear
scan then they proceeded to angiography, but otherwise were managed
medically -- and there was an 80% reduction in catheterizations! |
|
Catheterization
Laboratory |
So it's not like a trivial amount. I think we could
probably achieve more than 30%. But that goes to the question of
where CT is most useful. People have proposed it as a first line
agent for the evaluation of patients
with chest pain. Other people have said, well maybe it can be used
as a gatekeeper to the cath lab. And other folks have said, well
maybe it's a gatekeeper to nuclear. I think if it's used as a primary
test in patients without known coronary disease who present with
symptoms that are consistent with angina pectoris, that it can probably
be used as a first-line agent. And by being used as a first-line
imaging modality, thereby also serve as a gatekeeper to both nuclear
and to cath.
Q: To reduce the use of cath and nuclear and also be cost-effective?
Dr. Min: I think so. Everything that we know this far is that CCTA
is cost-saving. From single center studies to decision analytic
models to large multi-center albeit retrospective studies, we have
a fair amount of data to suggest that it is cost-saving and we
have absolutely no data to suggest that it is going to promote
more unnecessary testing or cost. I think everything that we have
thus far, until we are proven wrong, is that it is potentially
cost-savings.
I understand people's concern that it could
potentially be used in a way that does not help the patient. Just
to take a look at the
coronaries for the sake of taking a look at them is I think a poor
idea. But I don't think that anyone in the field is advocating that.
For its use in the evaluation of symptomatic individuals we know
that it diagnoses more accurately and excludes coronary disease more
accurately than any other noninvasive test we have. We know that
it has the ability to both exclude and identify obstructive or severe
coronary artery disease, thereby presupposing that we can identify
patients who can be stratified into a medical arm vs. an invasive
arm. We know that it prognosticates events, and we know that the
warranty period of a normal scan is long. There’s emerging
data to suggest that it's at least 5 years long – that, if
you have a normal CT angiogram, you're free for heart events for
a good 5 years, which is longer than other non-invasive tests we
have.
To say to somebody, "You have totally normal coronary arteries,
but we’re going to do some more testing on you” sort
of flies in the face of common sense. I guess I don’t really
understand where people are getting the idea that it's cost-increasing
or test-generating, because I don't think we have that data. I think
we have data to suggest the opposite.
Q: Some cardiologists I've spoken with, like Ralph Brindis of the
NCDR, expressed concerns that CT angiography will lead to more interventions
because you'll see a blockage and even though it might be flow-limiting,
it might get more people into the cath lab who maybe should be managed
in other ways.
Dr. Min: That's probably not the majority. If you take the low intermediate
to intermediate risk patient population, the majority of them don’t
have significant coronary disease. So that’s a patient population
you're sparing from cath. And in the minority of patients who have
obstructive coronary artery disease, what we know is that CT is more
effective at identifying obstructive coronary stenosis than stress
testing. And I think that's to be expected -- CT is an angiogram
and cath is an angiogram, so you'd expect that an angiogram and an
angiogram would correlate better than an angiogram to a non-angiogram.
If somebody presents with an 80% stenosis and chest pain and you
identify that with CT, and they progress to the cath lab, where they're
confirmed with an 80% stenosis, still with chest pain, then by conditional
probability, if you have a negative stress test, then that stress
test should be a false negative. That's just base theorem. So I don’t
see how the stress test helps you in that regard.
Q: Patients write into our Forum, "I had a nuclear stress test
and it showed blockages.” They use the terminology that "the
stress test shows blockages". As you are saying, it is not an
angiogram. Can you briefly explain to the lay population reading
this, why a nuclear stress test is not an angiogram.
Dr. Min: Sure, that's a great point. What the nuclear stress test
looks at is the relative perfusion of the heart, so it's all based
on the fact that if one area of the heart is not getting as much
blood supply, then you will see that. But it is a test that is designed
to look at heart muscle, not heart arteries. And it's the blockages
of the heart arteries that can potentially decrease blood supply
to the heart muscle.
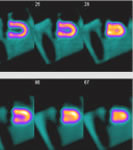
Nuclear Thallium
Scan |
|
So when you see an abnormal
stress test what you see is an indirect piece of evidence that
you may have heart artery blockages that are compromising blood
flow to that area of the heart muscle. We do stress tests for
the diagnosis of obstructive coronary artery disease indirectly
and for the prognostication of future events to help us re-stratify
and reclassify risk. An abnormal stress test may or may not represent
a blockage in the heart artery, but the goal of the stress test
is to try to indirectly identify that blockage.
The CT on the
other hand is just a direct picture of the artery and we can
just directly look into the arteries and see whether there
are blockages or not. That said, you don't get accompanying
information
from the CT about the heart muscle blood supply -- whether
or not the blockage is causing decreased blood supply to the
heart
muscle. |
Q: So the role for nuclear stress testing might be to see whether
or not the blockage shown by a CCTA might be causing a problem.
Dr. Min: Yes. I think that's people's concern, that if we're going
to do a test just to have to do another test, is that a problem?
I think it's a problem if you have to do a second test 100% of the
time. I think it's not a problem if you have to do a second test
7% of the time. And, at least from our lab, that's what I see. We
obviously have a selected patient population that either comes in
before or after the stress test but I would say the number of times
that I don't know exactly what to do with the patient, i.e. whether
or not the patient should go to the cath lab or go home on medical
therapy and may benefit from a functional imaging test is probably
on the order of 5-10%: a low number, not a high number.
Q: Another issue people are concerned about is radiation dose with
cardiac CT.
Dr. Min: That's a legitimate concern, but maybe one that is representing
or examining data that might be a generation or half-a-generation
old. There are numerous radiation reduction algorithms that can substantially
reduce radiation dose associated with CT and, without getting into
comparative details, CT certainly can be effectively implemented
with trivial radiation doses in comparison to say nuclear stress
tests. In our lab we use ECG dose modulation, we use auto modulation
of mA and we use prospective axial triggering in order to get radiation
doses that are really on par with background radiation doses from
walking around NYC for a year. So I guess the dogma is that average
baseline radiation exposure from just living at sea-level is approximately
3 millisieverts and that's approximately the doses that we generate
per coronary CT angiogram.
Is there an incremental risk of developing future fatal cancers
from ionizing medical radiation? I don't know but at least theoretically
I think there is. So it's responsible to practice under that thought,
because it ensures that medical practitioners reduce radiation doses
as much as possible. And that should be the goal. But when a patient
comes in, a 60-year-old man with chest pain, I think then you need
to weigh out the risks and benefits of an imaging test that includes
ionizing radiation and if the risk of future cancer is 1 in a 1000,
and the risk of future death from heart disease is 1 in 2 then I
think that you probably have your answer.
Q: Tell me more about these dose-reducing algorithms? Where did
these come from?
Dr. Min: I think you really have to tip your hat to the manufacturers.
They really made the technology such that we can do this. I think
the field should be applauded; particularly some in the field who've
examined the issues of radiation carefully. This technology has been
put forth by the industry, which was very cognizant of reducing radiation
to as low as possibly achievable.
Q: You are a member
of the Board of SCCT. The organization was mentioned in the New
York Times article that criticized CT.
Dr. Min: The SCCT was
unfairly characterized in the article. They claimed that SCCT
was an organization whose only aim was to promote CT angiogram
use, and nothing could be further from the truth. You have
to go to the web site to see what the mission of the SCCT is.
What we have now is a new test. I don't think it's going to
be the only test, but it's a new test and it's a darn good
one and its new in
our armamentarium of non-invasive testing. I think the SCCT's
role is to promote the responsible use of it; to promote education
of how to do it properly and with expertise; and to promote
the research endeavors that demonstrate the specific clinical
scenarios
where CT can be most useful. |
|

Society
for Cardiovascular
Computed Tomography (SCCT) |
Q: How do patients know that they are getting the right coronary
CT angiogram from the right place?
Dr. Min: I think they can ask about the interpreting imagers' level
of training -- and not only the number of coronary CT angiograms
that have been interpreted, but also where and by whom. I think that
training is probably the most important thing. There is certainly
a list of educational opportunities on the SCCT web site and the
vast majority of folks who are SCCT-endorsed are excellent. So to
have had proper training is important.
Q: Can you sum up the current status of cardiac CT?
Dr. Min: I think we're fighting against a few things. We're fighting
against a new era in imaging, which is being held to a higher standard
than prior imaging techniques have been held. We’re also
fighting against a process, where folks have a nuclear camera in
their offices and it's been a paradigm by which they have evaluated
patients with coronary disease for 20 years and it's tough to reverse
that. So there are multiple things that are ongoing that make this
a difficult battle: to try to get everybody to see the worth of
CT. But we've got a great test and now we just need to prove it
to people.
| This interview was conducted in August 2008 by Burt
Cohen of Angioplasty.Org. |
|





