Angioplasty.Org recently talked
with Dr. L. Nelson "Nick" Hopkins, Chairman of Neurosurgery,
Professor of Radiology, and Director of the Toshiba
Stroke Research Center at the University at Buffalo, State
University of New York. Truly one
of the pioneers in the treatment of stroke, as well as
the non-surgical therapies developed to treat both stroke and
carotid disease, Dr. Hopkins provides a unique perspective
into the growing area of cross-specialty and multidisciplinary
collaboration between and among medical specialities.
This three-part interview covers a range of topics:
- Part
One discusses the diagnosis and treatment of stroke;
- Part
Two deals with carotid artery disease;
- Part
Three discusses how imaging may impact future treatment,
and how reimbursement questions must be resolved for this
field to move forward.
|
|
 L. Nelson
Hopkins, MD
L. Nelson
Hopkins, MD
University of Buffalo
|
Q: The role of imaging has
always been critical in the detection and prevention of stroke.
In recent years newer
imaging techniques have become available, but would these constitute “a
sea change”?
Dr. Hopkins: Absolutely, yes. First we got
MR diffusion and perfusion studies which helped us to better differentiate
what tissues actually
had ischemia and infarction versus the areas that were that were
under-perfused, but not yet infarcted. So the MR studies helped us
to better understand the pathophysiology of stroke a little better.
But just in the last couple of years, with the new 64-slice CT scanners,
we’ve had a major advance in our ability to very quickly diagnose
and treat acute strokes.
With a 64-slice CT scanner you can get a CT scan,
which tells you whether or not the patient has a hemorrhage or not,
and you can get a CT angiogram very quickly with a relatively small
amount of contrast. 40-50cc will give you a reasonable CT angiogram,
as well as a CT perfusion study.
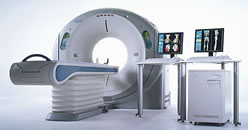
Aquilion™ 64-slice
CT scanner
(courtesy Toshiba America Medical Systems) |
|
And we now have been working
with Toshiba Corporation to develop some new algorithms using
the Vital Images Vitrea® workstation
to enable us to more accurately measure CT perfusion, cerebral
blood flow, cerebral blood volume and time-to-peak contrast accumulation.
Using these parameters we can very accurately and very, very
quickly
predict which areas of the brain are infarcted versus
those areas that are just ischemic. In a scan that lasts only
5-7 minutes total, we can get a pretty clear picture of what’s
going in the patient’s brain and it gives us very, very
clear directives as to whether or not we need to intervene. |
Q: So 64-slice CT is has implications in emergency
treatment of stroke?
Dr. Hopkins: Definitely. This has really
revolutionized the way we’re treating acute strokes. Because the big fear used to
be that we would revascularize an area of the brain that was already
dead and cause a major hemorrhage. If you reperfuse an area of dead
brain, then there is a significant likelihood that you’re going
to have a reperfusion hemorrhage. So these new imaging studies have
helped us to better understand which areas of brain are in danger
versus the areas of the brain that are already infarcted or dead
tissue. If we have a large area of infarcted tissue and dead brain,
then we usually do not try to revascularize that area of brain because
we’re not going to accomplish anything and we’re likely
to turn it into a hemorrhage.
The ideal candidate is, if we see a patient
with a major neurologic deficit and we see a large area of brain
at risk without a large
area of dead brain. That’s the kind of patient where we know
there is going to be a very major vessel occluded and we know that
we’ve got to get that vessel open if we’re going to prevent
that patient from having a major stroke.
Q: You’re talking about CT a
lot. Do you still use MRI?
Dr. Hopkins: MR and MRI and all the other variants
of MRI, perfusion, diffusion and so on, are still very, very important
to us. We get
much better resolution of brain tissue with an MRI. But in acute
stroke, where time is of the essence, we can learn as much as we
need to learn from the CT studies. MRI takes more time, and we want
to avoid that if at all possible.
MRI is still very important in the evaluation
of patients with impending stroke, or patients who have cerebrovascular
disease and who have
not yet had a stroke. MRI is extremely valuable. I don’t mean
to discount MRI. I just mean to simply say that in the acute phase,
we’re finding with the newer, higher-resolution, better, faster
CT scanners, we can learn what we need to know to allow us to make
a decision - whether or not we need to intervene and remove a clot
- much more quickly with just the one study, and so we’re not
using MRI so much in acute stroke anymore.
Q: Once you done the imaging, what are the tools
used to treat acute stroke?
Dr. Hopkins: There are basically two major
tools that we have available to us. One is intravenous tPA (tissue
plasminogen activator),
and that drug has been approved for a number of years for the treatment
of acute stroke. IV tPA can be very helpful. We find that it is quite
helpful in patients with lesser degrees of stroke. For example, if
somebody has a more minor stroke, that means you probably don’t
have one of the major trunk arteries shut down. And in that situation,
IV tPA can be very helpful. That means you’re dealing with
smaller branches that are probably occluded.
If somebody has a major stroke, with major
branch occlusion, then the likelihood of tPA giving you a good
result goes way down. If
you look at patients with NIH stroke scales, which gauge the degree
of severity of the stroke from 0-40 (0 is a normal patient and 40
would be a fatal stroke) -- if you have a stroke that’s NIH
scale 10 or greater, then the odds of recovery with IV tPA go down
a significant degree, like 75%. That’s because if you have
a major stroke with major deficit, then there’s probably a
major artery occluded and it’s not likely for IV tPA to be
successful in reopening a major artery. In that situation, we tend
to migrate more towards the use of a more aggressive approach, and
the other FDA-approved tool at this point is a clot retrieval device
called the MERCI Clot Retriever. So if we have a major stroke with
a major branch occluded, we would lean more toward removing that
with a clot retrieval device such as the MERCI device.
Q: And that’s done using endovascular
techniques?
Dr. Hopkins: That’s right. Usually
the femoral artery is used as an access point and micro catheters
are then navigated into the
intracranial circulation. And the clot retrieval device is then navigated
through the micro catheter into the clot, and is then used to capture
the clot and remove it.
Q: So surgical removal of clot isn’t
done?
Dr. Hopkins: It wouldn’t work. We’ve never had good
results with surgical removal of clots inside the brain, that is,
the kind of clots that form in arteries and cause acute stroke. First
of all, it takes too long to get there. Second of all, the brain
is very, very sick, and all the trauma of getting there seems to
be more than the brain can handle. So, the way to attack an acute
stroke where you have a clot that’s occluding a major cerebral
is to use the endovascular approach, using the vascular highway to
approach and then remove the clot.
(continue to Part Two)
| This interview was conducted by Burt Cohen of Angioplasty.Org. |
|



