
Craig
A. Thompson, MD, MMSc serves as Director of the Cardiovascular
Catheterization
Laboratory at the Dartmouth-Hitchcock
Medical Center in Lebanon,
New Hampshire and is Assistant Professor of Medicine (Cardiology)
at the Dartmouth Medical School. Dr. Thompson is board-certified
in Cardiovascular Disease, Interventional
Cardiology,
Vascular Medicine as well as Endovascular Intervention.
Dr. Thompson has stated that, as one of the oldest and
top-rated medical schools in the United States, Dartmouth
has been
training
cardiologists
in the use of intravascular ultrasound
(IVUS) and Fractional Flow Reserve (FFR) in order to ensure
that every trainee is versed
in the full line of diagnostic modalities available to improve
patient care.
Angioplasty.Org recently discussed with Dr. Thompson how
IVUS and FFR are impacting his practice,
especially with the new generation of drug-eluting stents.
|
|
 Craig
A. Thompson, MD
Craig
A. Thompson, MD |
Q: Intravascular Ultrasound has been around
for a while, yet only a minority of U.S. cardiologists is using it.
Why do you think that is and do you see the use of IVUS increasing?
Dr.
Thompson: I think the reason is that in most practices in the country,
IVUS traditionally has been somewhat cumbersome to use, in the sense
that a lot of the nurses and technicians and support staff that would
run an IVUS console for the physician may not have a high degree
of familiarity with how to run the system efficiently. So, there's
the perception that one cannot efficiently perform IVUS during the
course of a case, that it adds on the procedure time without necessarily
adding a lot of benefit.
I do think this perception is changing, and I
think that one of the drivers is that a lot of the academic thought
leaders continue
to adopt IVUS, and the reality behind this is that virtually any
time we investigate how to best perform intervention in groups
of patients, where IVUS is part of the decision algorithm, patients
do as well or better.
I think in the current environment, particularly
with drug-eluting stents and concerns about safety, is that part
of the milieu is
actually how to optimally deploy stents, and to optimally repair
a vessel. And IVUS is actually a very nice tool, in that regard,
to reduce ambiguity in terms of how well a stent is deployed, its
wall apposition in the vessel, downstream dissections or parts
of areas that are diseased but not appreciated by angiography,
that are not covered. IVUS reduces a lot of ambiguity, and I think
that the more that operators are familiar with interpreting IVUS
images, which has
been one of the other limitations through the years, and the more
efficient the IVUS systems are, I think the more that they will
be utilized.
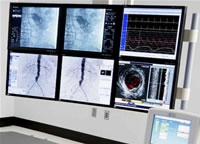
s5i Integrated
Display shows angiograms and IVUS images (courtesy Volcano) |
|
Also, I think the current
generation IVUS integrated table side systems really streamline
the process in terms of maintaining cath lab case and turnover
efficiency, and frankly, their edge detection and imaging chain
algorithms are becoming simpler to use, so that some of the
historic barriers to being able to use IVUS efficiently and
interpret the images and use that to possibly modify the intervention
are improving. I think just the simple integration of IVUS
systems at bedside is a huge benefit. It is tremendous. I think
its something that just cannot be adequately captured. But,
I think this is incredibly beneficial. Because of that and
the recurrent emphasis on having very good technique in stent
deployment and device utilization, I think IVUS is going to
have a resurgence. |
Q: Do you think that with
the coming 2.0
generation of
drug-eluting stents you will not need to use IVUS as much because
these new stents will be easier to deploy?
Dr. Thompson: No, I think
it still has a role. In fact, the more complex disease one is dealing
with, I think the greater relative value-add IVUS gives you. What
we've seen is that drug-eluting stents, generation 1.0 if you will,
was an enabling technology for us to address and approach disease
that would never been touched prior to drug-eluting stents, ever,
because of the severity of the disease, because of the durability
expectations, and so forth. So once drug-eluting stents generation
1.0 came along, we were approaching very complex disease. Much more
diffuse disease, and issues with calcification, and so forth. I think
both in terms of lesion assessment as well as an adjunct to performing
optimal intervention, IVUS has really flourished in this environment,
and I think that's part of the reason that we're seeing an uptake
in IVUS utilization.
When generation 2.0 comes along, I think
that's going to be an even more enabling technology because the
stents are
probably as good, if not better, in terms of efficacy, but the
improvements in deliverability again become something of a game-changer
in the
types of disease that most interventionalists can address. So
now you're getting stents to even more complex anatomy and more
distal
anatomy, and one has to really be that much more sure that the
job is done very well. So, even though the stents are improved,
I think
the fact is, what we're doing is continuing to move the change
in complexity of disease down the field. And I have very strong
bias
to believe that more complex disease state, the more value there
is to utilizing IVUS as an adjunct to intervention.
Q: What is your IVUS use and are there specific
cases or lesions where you do or don't use it?
Dr. Thompson: For my
group for coronary interventions, it is probably 20-25%. For me personally,
it's probably 60% -- IVUS is one of the things that I'm doing a lot
more of currently than I used to -- whether it's diagnostic assessment,
or as an adjunct to intervention. And basically, the logic sequence
is the same thing that I've discussed with you -- the more complex
disease, and the more I do, the more I'm inclined to utilize IVUS
to better reassure myself that the intervention is appropriate and
optimal for that given patient.
Q: What are the challenges,
with the fact that a lot of people don't know how to use or interpret
IVUS correctly,
and how have you been dealing with those challenges at Dartmouth?
Dr.
Thompson: Well, I think part of the challenge is to some extent the
shift in the technologies and being able to optimize the image. I
think one of the problems with IVUS historically is that the data
that one gets from utilizing IVUS is very rich, yet the amount of
this data that we're utilizing to understand what's going on in the
intravascular space and to make decisions is only a small percentage
of that. So, I think to some extent the challenges with simple image
acquisition and interpretation are how to best optimize the image
to understand what you're seeing, and then in terms of technology
development, how can we make the next generation IVUS better? How
can we go beyond grayscale IVUS and understand what's going on at
the tissue level? What do we understand about the lumen-blood interface?
How can we use IVUS to better understand the three-dimensionality
of the vessels: to take a 2-D image and turn it into a 3-D information
system?
I also think that experience begets experience, with IVUS, I think that's really the key, for me: the more IVUS we do, the better we get at it. We get better at performing it quickly and efficiently. We get better at understanding which lesions or which interventions are best suited for IVUS as a helpful additional modality. We get better at image interpretation, and understanding what we're seeing. And we get better at optimizing the images, and getting the most information that we can from an image, rather than it being fuzz.
| To some extent, we have
a little bit of a problem with IVUS literacy in this country.
A lot of people can look at IVUS images, but the amount of
information that one can factor into a decision-making process
to take care of a patient may be variable from center to center,
or individual to individual. What we're trying to do in training
our fellows, for instance, is to establish some systematic
approach to looking at IVUS and understanding IVUS systems,
just as we would systematically look at an electrocardiogram
when we take care of a patient, that there are certain aspects
that you need to categorize when you're looking at images,
that should be very similar from patient to patient, so that
you reduce the amount of variability in images that you acquire. |
|

Dartmouth-Hitchcok
Medical Center |
Q: In his
interview with Angioplasty.Org,
Antonio Colombo said that even when he doesn't use IVUS, he still
has an IVUS
mind set in
terms of imagining what's going on in the vessel, optimal expansion,
etc. Do you think there's validity to that? Do you see that happening
in your practice?
Dr. Thompson: I think without question that is true.
Does experience with IVUS, doing IVUS-based interventions, for instance,
does that inform your practice for non-IVUS cases? I would say it's
absolutely true. I think there are little wrinkles that you see in
stents, for instance, that by angiography don't look that bad, but
that your experience seeing similar cases with IVUS would suggest
that, for example, that its
an under-deployed stent. That there are small hazy areas at stent exits, for
instance, that are less impressive by angiography, but that you realize with
experience from IVUS may represent an edge dissection. I'm very, very convinced
that utilization of IVUS informs practice in a positive manner for cases in which
you do not utilize IVUS.
Q: You're also working with other technologies including FFR. Have you found that of value?
Dr. Thompson: I think there is value to FFR. It's interesting. In our practice some of my partners, when there's lesion ambiguity, some of my partners gravitate more toward FFR to better understand the hemodynamic significance of a lesion, and some of my partners may gravitate more towards IVUS. I think they're both helpful technologies, I think there's a value-add to both technologies. I think the issues specifically with FFR that one has to bear in mind, in distinction with IVUS, is that they're both probably good technologies to assess intermediate to severe lesions in a patient with stable coronary disease, but I'm less convinced that in patients who present with unstable coronary syndromes that FFR adds as much value, to me, as IVUS does. Because a lot of the validation sequence behind FFR is based on patients with stable disease, and understanding how in context both with patient outcomes, and with stress imaging studies. IVUS on the other hand, I feel, gives me better information of structurally what's going on with the intravascular space, and while you could certainly challenge the data chains that exist behind IVUS utilization in unstable syndromes, I do feel for me it informs my practice in that patient sub-set as well. I find, for me, IVUS has much broader utility than FFR, but I think FFR is certainly a helpful technology in intermediate lesions.
Q: Have you found that tools
like FFR and IVUS can help you triage a patient, as to whether
an intervention
is even needed, or perhaps deciding, Maybe this is a bypass candidate?
Dr.
Thompson: I think they do. At least in the more proximal epicardial
coronaries, using either IVUS or FFR can be informative about who
is approachable
and who is not, at least in the stable patient. And I do think that
there's value to this. I'm hopeful that, as time passes and as technology
improves, that we might be able to use these or other modalities
to more intelligently make decisions based on adjunct and imaging
tools, either as patient vascular risk profiling or as lesion specific
risk profiling, and I think IVUS will play a strong part in that.
Q: Is this in the issue of plaque characterization,
and being able to identify so-called vulnerable plaques?
Dr. Thompson:
Exactly, and hopefully we start to get some information back
on this, at least in concept. Its not yet there, but it's under
intense study, and it's certainly a reasonable area to investigate.
But
again, I
think there's more available information coming back from IVUS,
and it's how to best optimize, and to include that in the decision-making
process, whether it's best to do an intervention, or not to do
an
intervention, or how to do an intervention.
Q: Even in the S.T.L.L.R. study, which was
done angiographically with QCA, 2/3 of the stents studied were under-deployed.
Do you think this is pretty representative? Can IVUS use solve part
of this problem? And from a training standpoint, what should a cardiologist
do in order to be able to learn IVUS?
Dr. Thompson: I would say that
S.T.L.L.R. is probably representative of conventional practice with
drug-eluting stents. In order to more optimally deploy the stents,
high pressure balloon dilation is obviously very important, but IVUS
has a role in this. How do you go back and re-learn IVUS if you're
not doing it frequently? Well, there are IVUS courses and sub-courses
at a lot of the major national meetings, at American College of Cardiology,
I2, TCT, there are dedicated courses through ACC in which you can
re-train or re-calibrate your eye with IVUS. The companies that manufacture
and sell IVUS have programs for physician education and bringing
physicians for proctorships or going to high-volume IVUS labs and
learning, so I think there are mechanisms that industry is trying
to support in order to better learn IVUS.
I think that the national
meetings, and through industry support, are two of the major
mechanisms. After that, one learns by doing, as again I think
success begets
success, and the more IVUS you do, the more comfortable you become
interpreting the images. So, it's just a combination of trying
to go back for additional education, and practicing.
This interview was conducted in February 2008
by Burt Cohen of Angioplasty.Org.
|





