 |

|
 |

Jennifer Tremmel,
MD
is Director of Transradial Interventions at
Stanford Medical Center and Clinical
Director of Women's
Heart Health at
Stanford Clinic. Dr. Tremmel
studies sex differences in cardiovascular disease. She is
an Interventional Cardiologist who also trained in Preventive
Cardiology. In her clinic she cares for women who are at
high risk for coronary artery disease, women who have symptoms
concerning for heart disease, and women who already have
heart disease. She has a particular interest in women who
present with symptoms of heart disease, but are found to
have "normal" coronary arteries on angiography. Her current
research investigates whether women presenting like this
are more likely than men to have coronary abnormalities that
cannot be detected by angiography alone, such as endothelial
dysfunction, diffuse deposition of plaque, or microvascular
disease.
Dr. Tremmel received a B.S. in Psychology and an M.D. from
the University of Iowa. She did her Internal Medicine Internship
and Residency at Dartmouth-Hitchcock Medical Center, followed
by a Master's Degree in Epidemiology
at the
Harvard School of Public Health. She completed her Fellowship
in Cardiovascular Medicine and Interventional Cardiology
at Stanford University Medical Center, where she was also
a Postdoctoral Research Scholar at the Stanford Prevention
Research Center. For more about the transradial approach, visit our Radial
Access Center. |
|

Jennifer
Tremmel, MD,
Director of Transradial Interventions, Stanford Medical Center
and Clinical
Director of Women's Heart Health
at
Stanford Clinic |
Q: Why did you decide to start using the transradial
technique for angioplasty?
Dr. Tremmel: Well I had an epiphany. It had bothered me that my patients
were periodically having bleeding or vascular complications. It certainly
wasn’t happening at a higher rate than anyone else’s
but whenever it happens it's an unfortunate situation: the patients
don't like it and it certainly can lead to a lot of morbidity and
mortality. Being someone who does research in sex differences, I
knew that my women patients were more prone to having bleeding complications.
I could say to them, "Well, you're more prone to having this
problem," and they always looked at me like, "So what are
you going to do about it?" and I couldn't really give them a
good answer. The answer certainly was not vascular closure devices
because those don’t decrease bleeding complication rates. You
try to improve your technique as much as you can but you still have
these complications.
This was always in the back of my mind
and one day I saw an article which said that both sexes have
significantly lower bleeding rates
with transradial intervention, particularly women, because they
have higher bleeding rates at baseline. So when I saw that, I was
like, "This is it!" It seemed like the answer to taking
care of these vascular complications. I felt a real obligation
to figure out a way to lower bleeding complications just because
I'm a women's heart health specialist and that's my job: how do
I improve the outcomes of the women that I take care of? In my
mind, transradial was the answer.
Q: Why do women physiologically have more bleeding complications?
Dr. Tremmel: No one knows exactly. I think it's multifactorial.
Some thoughts are that women’s vessels are smaller, so
when people are trying to get access, they may use more needle
sticks, or they may be more likely to experience posterior wall
sticks, where the needle goes through the vessel. There also
are some thoughts that women wind up being overdosed with medications
because their size is smaller. But even if you dose them properly,
women still have higher bleeding rates than men. There also are
some thoughts that their vessels simply may be more fragile.
We know they're more prone to getting things like dissection
and that sort of thing, so there may be something about the hormonal
milieu that makes their vessels more fragile and prone to bleeding.
Nobody knows exactly why. If we knew exactly why, it might help
us decrease the gap.
Q: You mentioned that vascular closure devices don't really decrease
the bleeding complications.
Dr. Tremmel: Vascular closure devices decrease the amount of time
that somebody has to lie flat after a procedure. They can get up
sooner. There's a lot of patient convenience. But anybody that
sells you vascular closure devices will be honest with you that
they don't decrease vascular complication rates. We know that from
quite a bit of literature.
Q: Patients write into The
Forum on Angioplasty.Org about the problems and concerns surrounding
their groin puncture
and its
healing – less so about the stent in their coronary artery.
Dr. Tremmel: Right. That's what people remember about their procedure:
the time afterward when somebody was pressing on their groin for
four hours, or they were lying flat and their back was killing
them. They take away a lot about how their whole procedure went
based on how the post-procedure part went. You could have done
the most beautiful complicated angioplasty in the world, but they
don’t care if they have this giant bruise down their leg,
or they're getting transfused.
St. Vincent's
Transradial Training
Course in NYC |
|
Q: Once you made the decision
to do radial interventions, how did you go about learning it?
Dr.
Tremmel: It was one of those things where, if the student is
ready, the teacher will appear. It was in my mind, OK, now
I need to learn how to do radials, and it was just kind of
luck -- for some reason the Terumo rep came through our lab
and said "I have some training
available -- would you be interested? And I said, "Yes!
So
I took the next plane to New York -- I did the St. Vincent's
transradial course in New York that Terumo hosts. It was
a day-and-a-half and I left feeling very comfortable and
confident
that I could go back to my institution and start doing them.
And I did. |
I chose a specific
nurse and a tech so I would have the same people with me
as we were starting
to learn and I wouldn't have to go through it with everyone
and people wouldnt be all upset -- because anytime you try
to do something new, people are like, Oh my God, what are
you doing? So they scrubbed in on all my cases and we figured
out how we were going to set up the patient and what equipment
we needed. The nurses in the cath lab got used to what we were
doing and what it looked like afterward. I also had one nurse
in the holding room who was specifically assigned to my patients.
I used the TR Band and learned what it was about and we
did that for a month or so. There was certainly a lot of
buzz around
the lab like, What are they doing? |
|
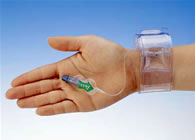
TR
Band™ Radial Compression Device (courtesy Terumo
Interventional) |
So at that point I held an in-service for
the whole lab. And I asked my nurse and tech to start teaching
everybody else to do
their parts. And everyone got pretty comfortable with it. Then
we trained the floor nurses, so that when patients come out, they
go to the holding room and then go to the floor, and the nurses
knew what to do with the wrist bands. It turns out that it's much
easier to deal with. The nurses actually love it because they don’t
have to hold any groins. And the patients are very autonomous.
They can get up, and go to the bathroom and they don't need bed
pans and all of that.
Q: So you did the in-service only a month or two after you returned
from New York? It was really see one, do one, teach one.
Dr. Tremmel: Yeah. I was really motivated to do this. It rung so
true to me that I really wanted to make it work. They had told
me at St. Vincent's that it's best if you try to do it 100% of
the time, as opposed to trying to pick and choose. That made sense
to me and so I came back with a plan that I'm going to do this
100% of the time. When I started doing it, some would work and
some wouldn't and I didn’t always know why it wouldn't. I
would say it's spasm but I didn't know if it was spasm. So if it
didn’t work we always had the groin prepped.

Stanford
University Medical Center |
|
We're a teaching
institution so I also did radials with my interventional
Fellows -- once
I felt comfortable, I let them start learning. I did my training
in June and by mid-December, when I looked back, I realized
that they had become exceptional at doing this.
And from mid-December
until this week (April 2009) we didnt have to go to the groin
once! So weve had almost a four month period of success. The
learning curve's fairly long which everyone always says. It
took us about six months to become really really good at
it, but then
we got really really good at it! We just kept at it. In the
beginning it was frustrating sometimes and it was tiring. |
Interventionalists like to get things done and when we're
really good at something it's nice to just go in and do it and
in five minutes you're done! So it's hard to step back and say
okay, I'm going to do something new and I'm going to go through
this. But in the end, it really paid off. And it didn't take that
long. It's all now a past memory.
Q: The rest of the world uses the radial approach 40-50% or more,
and the U.S. is way behind, in the low single digits -- you even
had trouble finding training. What are the major roadblocks to
the adoption of the radial technique? Is it motivational or is
the problem that there's just not enough training out there?
Dr. Tremmel: I think it's a lot of things. The initial thing is
that learning to do interventions is really an apprenticeship.
So you learn from your mentors and they teach you what they know.
That's how I was trained.
Secondly, I would say that, for the most
part, it works great through the groin. When we have bleeding
complications, we do fine
with most of them. Rare cases can be lethal, however, as you know,
so retroperitoneal bleeds can be lethal, particularly if people
who are not paying attention. But with bleeding complications we’ve
kind of said, "Well, this is part of angioplasty..." and
we've accepted it, when in fact maybe we don’t need to accept
it -- and certainly not at the rate that we have it. It's kind
of like stent thrombosis -- we went through the part where stent
thrombosis was terrible and now we're getting used to it. It doesn't
happen very often but, when it does, it can be awful. Certainly,
if more people were bleeding every single day, then they would
be looking for other options.
I think third, you have to learn something new, and if you're
out of the learning phase or far out from Fellowship, you just
may not want to be learning something new. You may feel pretty
good about what you're doing.
Fourth, I think is training. You're right. At this point it's
still a little bit harder to find training. You've got to get time
off to go do it. So you would have to be motivated to do the training.
And then I would say fifth is that the
patients at this point still don't know about radial that much.
Or they don’t know
there are options, so there's not feedback from the patients, such
as, “I would actually prefer that you do it through the wrist.
Oh you don’t do it through the wrist? Well maybe I'll go
somewhere else.” So I think that's an issue. Once people
find out that you do it that way and maybe they've seen an article
or something, once they hear that there's another way to have this
done and that their bleeding risk may be lower and that they can
get up and walk right afterwards, they may come asking for it.
And I can tell you that's going to motivate a lot of interventionalists
to change because their patients want that.
Then there's actually another reason: the
equipment we use. I think the equipment is getting a lot better.
I know people tried
starting radials in the past and ran into a lot of frustration
because wires and sheaths were harder to get through. Certainly
the stuff that we have available now, hydrophilic wires and hydrophilic
sheaths that slide through and these radial-specific catheters
that can do the right coronary and the left coronary with one catheter,
I think that, as the equipment improves, cardiologists will be
more motivated too, because it will be simpler, they'll have less
obstacles in mastering the technique. I think there's some remembrance
from the older practitioners that it didn’t go very well,
that it was hard to get stuff in and that sort of thing.
Q: In the not-so-distant past, catheters and sheaths had to be
larger French sizes because the balloon profiles were bigger.
Dr. Tremmel: Right! Everything is smaller now. And there is certainly
misinformation. Yesterday I did a lady who is 37 kilos. That's
the smallest lady I’ve ever done. She's 81 lbs. And I did
it through her radial artery. She had a beautiful return when we
got in. I was shocked. Her wrist was so tiny, but we had no problems
with it. And that was part of the doing 100% and not picking and
choosing -- because you really don’t know. You automatically
would say that all the big guys are going to be easier -- which
is in general the case, but this teeny little woman, no problem.
And she was certainly at high risk for retroperitoneal bleed from
the groin, because we know that the majority of people that bleed
are women. The studies that I did with my colleagues showed that
73% of the retroperitoneal bleeds were women. And also small body
surface area. So, little women, high risk for a retroperitoneal
bleed.
Q: What has been the impact on your practice and with your colleagues,
now you're doing all these cases radially?
Dr. Tremmel: The impact? Certainly we don't have any bleeding complications.
It was funny, the Fellows yesterday were like "You never have
any complications" and I said "I know. Isn't it nice?" So
that's an impact. There are more people who are requesting to be
done this way: patients and referrals. The big thing is having
referrals: people specifically send their patients to you because
they would like it done this way. Periodically I get called up
to the lab, "Can you come help do this radially because we're
having groin problems?” So it's a service that I've been
able to provide that we didn’t have before. And my colleagues
have said that we should disseminate this and we should all be
learning it. That's really what I was hoping for -- that they also
would want to start doing radial.
Q: You’ve recently given presentations to some managed care
groups – are there economic implications with the radial
approach?
Dr. Tremmel: I've talked to them about cost-effectiveness. Overall
radial comes out to be less expensive than femoral. Particularly
if you're using closure devices with your femorals -- it's a lot
cheaper to do it radially. Particularly if you add in things like
nursing afterward and hospital stays -- all those things become
shortened. And fewer complications are always less expensive. We're
in an era now of healthcare reform and these are the issues that
are really going to come to the forefront and I think hospitals
are going to be looking to find ways of having people do interventions
radially, if they can, because it will lower their costs and complications
and stays.
Q: Do you think meeting organizers from ACC to SCAI to TCT should
be putting more emphasis on training cardiologists in radial during
those meetings, like with live cases, etc.?
Dr. Tremmel: Those would be great forums for training courses because
you can be trained quite quickly, at least enough to have confidence
to go back and try it. We're all interventionalists, so we know
the basic technique of getting into an artery and advancing sheaths
and advancing catheters. You just need some sense of how to do
it in this particular way. And then you have to go back to your
institution. A lot of it is trial and error, knowing when you need
to stop, and when you can keep going. And your confidence grows
as you do more of them. And you don’t need days and weeks
of watching somebody or having them watch you. When I did Dr. Coppola's
training course, I think I got to do a stick three times, and that
was really helpful, having somebody right there with me. But I
certainly think that ACC and others could give some information
be it videos or simulators or watching live cases that would enhance
people's learning. People walk away from these meetings with the
sense that “this must be important because it came up a lot
and it got a lot of press”, so they're thinking, “I'd
better learn about this." That's why we all go to these meetings.
Q: Any final words of advice to cardiologists who don't now practice
the radial technique?
Dr. Tremmel: Try it, you'll like it!
This interview was conducted
in April 2009 by Burt Cohen of Angioplasty.Org.
|





