 |

|
 |

As part of its
ongoing series of interviews with physicians who practice
the transradial approach for angiography and angioplasty,
Angioplasty.Org recently talked with R. Lee Jobe, MD, Chairman
of Invasive Cardiology at Wake
Medical Center in Raleigh, North Carolina.
In this interview Angioplasty.Org discusses with Dr. Jobe
why the the transradial approach is under-utilized in the
U.S. and how it can lower complications and increase patient
satisfaction. For more about what the transradial approach,
visit our Radial
Access Center.
Q: For most patients in the U.S., catheter
access for an angiogram or angioplasty is done through
the femoral artery in the groin. What is radial access
or the transradial approach, using the radial artery
in the forearm?
Dr. Jobe: The transradial approach is an alternative access to the coronaries,
from the radial artery rather than the traditional femoral artery. We
have developed and used transradial access to try to reduce the complications
and improve patient satisfaction with the procedure.
|
|

Dr. R.
Lee Jobe
of Wake Medical Center
Raleigh, North Carolina |
Q: What are the complications in
the femoral approach that are being reduced?
Dr. Jobe: From the femoral access, we run into problems with bleeding, both
from the artery out to the skin, and from the artery backwards into the retroperitoneal
space, because the femoral artery, depending on where exactly the needle stick
into the artery is, is not easily compressible when we pull the sheaths and
catheters out. In addition, some people tend to carry a little extra weight
down around their waist and thighs, and there can be a significant amount of
extra body tissue overlying the femoral artery, making it deeper and more difficult
to gain control of the artery for pressure when you pull the catheter out.
The radial artery is just underneath the surface
of the skin in virtually everybody, and is easily accessible with
catheters. The radial access is easily compressible with fingers
or any of several support devices that are available.
The other advantage that we look at is that people
who have had femoral artery access often are limited to bed rest
for somewhere between two to six hours after the procedure. From
the radial access, patients are literally ambulatory immediately.
So there's none of the discomfort or complications that are associated
with the prolonged bed rest after femoral access.
Q: Are there other complications,
besides bleeding, that are lessened by using the radial approach?
Dr. Jobe: Most all of them are bleeding-related in one way or another, either
hematoma, femoral artery pseudoaneurysm, arterial venous fistula between the
femoral artery and femoral vein, and retroperitoneal bleeding. In some of the
larger patients, there's also a risk of cellulitis or skin infection from femoral
access. There's virtually no risk of cellulitis or skin infection from radial
access,
Q: We get patients writing into our
Forum who have had femoral access and have wound up with some
level of disability post-procedure. They find that their leg
is weak, they're limping, and they've been diagnosed with some
sort of nerve trauma or nerve damage that has occurred.
Dr. Jobe: Well, the femoral nerve does lie right beside the femoral artery,
and it is possible to damage the femoral nerve either transiently or permanently
with catheter access. In addition, the femoral artery is the largest and essentially
sole blood supply down to the leg. So, if a clot were to form in the femoral
artery at the catheter site and travel down the leg, there could be a significant
ischemic problem in the leg from embolization.
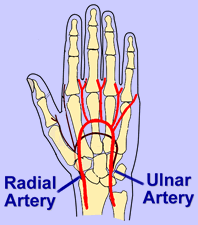
By the nature of the patients that we select
for radial artery access, there's dual blood supply to the hand
through the ulnar artery, which we carefully look for and document.
By this dual blood supply, even if the radial artery is totally
occluded after our procedure, there will be no distal vascular
complications, because the hand is protected by the ulnar artery.
Q: Femoral artery complications
are quoted at around 3%, but most cardiologists we've
spoken to agree that it's higher, if you take into
account
what are considered “minor” complications. Are
complications
really lower with
radial access, or is it just a different kind of complication
that occurs?
Dr. Jobe: Oh, it's substantially lower than that. With radial access, we do
several hundred cases a year here at our institution, and our complication
rate would easily be less than one half of one percent.
Q: What is the percentage of cases
that you do radially?
Dr. Jobe: I do about 1,200-1,300 diagnostic procedures a year. I do approximately
400-420 interventions a year. 50-60% of those would be radial, including the
diagnostic.
Q: Some cardiologists assume that
you do radial only when you can't do femoral -- for reasons
of
obesity,
or where there's disease in the femoral artery. Is that the
way you approach it?
Dr. Jobe: No. Actually, what we're finding is that, rather than viewing radial
access as a bail-out when the femoral won't work, the better approach is to
look at the radial access as the primary access point, and use the femoral
only when the radial is contraindicated. So, I think it just takes a little
bit of change of mind set. Rather than looking at the radial as the backup
access, look at it as the primary access, and then use the femoral as your
fallback
approach.
|
|
Q: When you look at a patient,
how do you judge whether they are candidates for radial
access?
Dr. Jobe: We test for collateral blood flow to the hand. The hand has dual
blood supply beginning just below the brachial artery where it bifurcates into
the radial and the ulnar arteries. They meet in the palm or arch in the hand.
So, what we have to see before we think a patient is a candidate for radial
access procedures is that there's adequate flow down the ulnar artery, and
that it goes through the palm or arch, completely all the way around to the
thumb.
The basic test is some version of the Allen test. We occlude
both the radial and ulnar artery. We'll see that the hand
will blanch completely, and then we release the ulnar artery,
and through one mechanism or another -- either visual assessment
of the return of blood flow to the hand, or pulse oximetry
on the thumb -- we will document that there is complete collateral
circulation to the entire hand through the ulnar artery only. |
Q: What are the cases in which you
don't do radial as primary?
Dr. Jobe: If there's not collateral circulation to the hand, we won't go radial.
We also find that many patients who have had previous coronary artery bypass
grafting are not optimally done via the radial approach, especially patients
who have had the left internal mammary graft utilized.
Q: The radial approach has been around
15 years or so, but in the U.S. patients don’t hear about
it very much. Is it that there’s resistance to it in
the U.S.?
Dr. Jobe: In the Netherlands, the penetration for radial procedures is approximately
2/3 of the procedures done. In France, 30-40% of all procedures are done radially.
In Japan, the penetration is similar, approximately 40%. And in the United
States, when we poll our interventional cardiologists we find that it’s
less than 2%.
I don’t think it’s resistance, I
think it’s lack of motivation to acquire the procedure. In
European and Asian centers, physicians and hospitals are not limited
by reimbursement. If they can do an intervention successfully and
have the patient be ambulatory, those patients can be discharged
and go home the same day. With the femoral approach, it is virtually
contraindicated to send the patient home the same day, regardless
of whether any femoral-type closure device is used. But with the
radial access we literally can ambulate the patients immediately
[allow them to stand up and walk]. Discharging them several hours
later is not a problem.
But in the United States current Medicare/Medicaid
reimbursement actually penalizes the hospital if a procedure is
designated as an in-patient procedure, which coronary stenting
is, and if the patient is sent them home the same day as an out-patient
-- the hospital is actually penalized for that rather than rewarded.
So there has not been a financial incentive for people in the United
States to pick up the procedure. I think if it were reimbursed
equally as an out-patient or ambulatory procedure, hospitals would
strongly encourage their physicians to do it because a certain
number of patients who have coronary interventions done could be
done as out-patients and discharged home the same day, which would
free up hospital beds.
Q: So you’re saying that one
of the big reasons for keeping patients overnight has little
to do with their heart disease – it has to do with the
healing of the femoral artery puncture that is made for catheter
access?
Dr. Jobe: Right exactly.
Q: Do you see the reimbursement issue
changing?
Dr. Jobe: I do. CMS is, of course, accepting proposals for getting changes
to their reimbursement models that may help them save money. We have written
them a proposal to use our institution as a demonstration site for ambulatory
coronary stenting from the transradial approach. Under the demonstration site
protocol, the hospital would not be penalized for doing these patients as out-patients
and through a program like this we could demonstrate to CMS that selected transradial
coronary interventions could actually end up saving the health care system
significant amounts of money by allowing us to do patients as out-patients.
Q: In your own practice in North
Carolina, what have been the major advantages of using
the radial approach?
Dr. Jobe: Primarily, the reduced risk of femoral bleeding
complications -- the reduced risk of vascular complications,
including distal embolic events. But
the primary thing that really drives this for us is increased patient satisfaction.
They find that it’s so much more comfortable to be able to sit up in a
chair immediately following their procedure.
When they’ve had femoral access,
they’re restricted to bed rest for 4-6 hours because of the risk of bleeding
from the femoral artery, and if they need to use the bathroom they’re restricted
to bed pans.
But from the radial approach, they’re up and ambulatory immediately.
They can sit up, they can eat, they can go to the bathroom normally, if they
have problems with chronic back pain or muscular skeletal disorders, they can
work with those immediately. We just find that once a patient has had a radial
access procedure, they really don’t ever want us to go back to the femoral
again. |
|
Dr. Jobe in the cath lab |
From a physician’s standpoint, we find
that it’s a unique calling card that separates us. We think
that it helps give us a little bit of a competitive advantage,
because we are the only group here doing a significant number of
radial access procedures. And our patients like to go back home
and talk to their friends and family and when they say they’ve
had their catheterization procedure done, they point to their wrist
and they say, “Oh, it was Dr. Jobe or it was Dr. Mann”,
and it’s just one more thing to talk about, one more thing
that gets our name thought of a little more frequently. It’s
just one more feature that makes our practice unique and memorable,
both to our patients and to our referring physicians.

Wake Medical Center,
Raleigh, North Carolina |
|
Q: How did you get involved in this? When
did you do your first radial procedure?
Dr. Jobe: Dr. Tift Mann, here at Wake Heart, is one of the
major proponents of transradial procedure. He learned directly from Dr. Kiemeneij
in
Amsterdam,
and
as soon as I joined Wake Heart, within the first week I was doing transradial
procedures as well, as soon as Dr. Mann showed me the technique.
|
Q: That brings me to training. You
learned in a one-on-one mentoring situation. Today how would
a cardiologist who doesn’t do radial go about learning
how to do it, what is the learning curve?
Dr. Jobe: I’m glad you brought up learning curve, because
there is a learning curve to the procedure. We think it’s important
that the first 100-125 patients people select, when they’re going
to bring transradial to their practice, be patients who are likely
to
be easy transradial
cases. Middle-aged men with large radial arteries make very easy
transradial access. We find that elderly patients, especially elderly
women, are very likely to have tortuous subclavian, tortuous innominate
arteries, and tortuous ascending aortas. And patients who are short
tend to have very short ascending aortas. Those are some things
that make the access a little more challenging, and those types
of patients should perhaps be reserved for later on in somebody’s
experience.
We think the way to gain experience is a three-pronged
approach: first, attending one of several training sessions that
are sponsored at several hospitals throughout the United States;
then, a couple of companies have developed computerized simulators
where the physical approach to transradial, manipulating catheter,
catheter selection, accessing the radial artery, can be practiced
in a simulator setting, is important; third is to have a mentoring
process. They should invite somebody who’s very experienced
to come to their center and spend a day or two with them while
they’re doing their own cases in their own center, and offer
advice and critique the technique within their own hospital.
Q: Is there a problem using any devices
with the radial approach?
Dr. Jobe: We typically use 6F catheters, and anything that can fit through
a 6F catheter will work via the radial access. We’ve used rotablators,
up to a 1.5mm burr. IVUS can be successfully done through the radial, AngioJet
rheolytic thrombolysis can be done through the radial. We find that kissing
balloon, kissing stent techniques all can be done through the transradial with
6F catheters quite successfully. You cannot put in a balloon pump from the
radial access, so that is pretty much the absolute contraindication.
Q: If you’re just doing diagnostic
caths, can’t you do these as outpatients, even with the
femoral approach?
Dr. Jobe: Yes. But in the femoral approach, if we’re going to try to
send them home the same day, most of the time we’ll use some form of
closure device, and the closure devices, of course, have their own complications
associated with them including infection, including embolization of the closure
device material, including occlusion of side branches. There is no closure
device needed with transradial.
Q: How does it work when you pull
the sheath out?
Dr. Jobe: We pull the sheath out when we’re done, regardless of the level
of anticoagulation, and we use a radial artery support device. So we find that,
for example, if we have an emergency coming from the emergency department or
transferred in from an outside hospital, who maybe has received full thrombolytic
therapy, or is aggressively anticoagulated with heparin and a IIb/IIIa inhibitor,
we specifically look at those patients for transradial access just because
the bleeding complications from the access site will be lower.
Q: How quickly
are you able to achieve hemostasis and stop bleeding?
Dr. Jobe: In diagnostic catheterizations where we do not provide significant
anticoagulation, we’ll maintain pressure with a radial artery support
device for 20-30 minutes. Then it’ll be loosened and removed.
In a fully
anticoagulated intervention, we’ll leave the device on for about an hour
before we start loosening it and removing it. And we have all of our staff
well in-serviced on how to assess the radial artery for adequate hemostasis. Q: And all this time the patient
is still ambulatory?
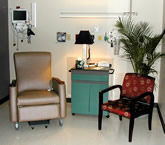
Dr. Jobe: Right. Our transradial recovery area doesn’t have stretchers,
it’s got chairs!
Q: So to sum up the major advantages
of the radial approach?
Dr. Jobe: I think the major selling points on transradial and the reason that
we believe it in so much are the virtual elimination of vascular complications,
the increased patient comfort and satisfaction associated with it.
This interview was conducted in July 2007
by Burt Cohen of Angioplasty.Org. |
|
 |
 |
|







