 |

|
 |

Dr. Mauricio
G. Cohen is Director of the Cardiac Catheterization Lab
at the University of
Miami Miller School of Medicine. A native of Argentina,
Dr. Cohen joined the University of Miami in September
2008 after five years at the University of North Carolina
School of Medicine
where he was an assistant professor, as
well
as Associate
Director
of the Catheterization Laboratories and Director of
the
UNC Healthy
Heart Latino Initiative, providing health
care services and outreach to the growing Latino community
in
North Carolina (ed. note -- this interview was
conducted just prior to Dr. Cohen's move to Miami.)
Previously Dr. Cohen studied interventional cardiology
at Duke University
Medical Center, having been honored with the
Latin American Society of Interventional Cardiology Duke
Scholarship in 1997. After completing his training, Cohen
returned to Argentina as clinical research director in interventional
cardiology at
the Hospital Italiano de Buenos Aires, one of the major referral
medical centers in South America.
For more about the transradial approach, visit our Radial
Access Center.
|
|

Mauricio
Cohen, MD, FACC
University of Miami Miller
School of Medicine |
Q: When and why did you start using
the transradial approach?
Dr. Cohen: I originally trained in Argentina. By the time I was finishing
my general cardiology training, the interventional group at my
hospital was doing a randomized study allocating patients to radial,
brachial and femoral access. That was in the mid-'90s, when very
few people were actually doing the radial technique. Some patients
were having radial diagnostic catheterizations, and that was working
very well. But all interventions were done via transfemoral access,
because the interventional equipment would not fit in a 6F catheter.

University
of North Carolina
School of
Medicine |
|
Then I had the fortune to
come to the States and train at a great institution such as
Duke. But I noticed the epidemic of obesity that was affecting
this country. After a few years, when I became faculty here
at the University of North Carolina in Chapel Hill (UNC), I
noticed that doing the morbidly obese patients always posed
a significant risk.
We were getting a number of patients, who
had been referred for bariatric surgery. And all the required
imaging studies and stress-testing were not optimal because
of the large volume of these patients. |
So
many of these patients were being referred to cath instead, and every
time we had to do a femoral approach in them, we were always afraid
the patients would bleed and/or would have a complication. And by
the time we realized the patient was having a bleeding complication,
the patient probably bled half of his volume and the patient might
be in hypovolemic shock and sometimes it might be too late. We also
understood that bleeding complications were correlated with very
poor outcomes, in the short and the long term, especially in patients
who were undergoing PCI or had other co-morbidities.
A landmark situation was a
patient where we had to use a vascular closure device. The
ones that I was most familiar with were the Angio-Seal and
the Perclose device. We had had a complication at UNC with
a Duett device, which consists of a balloon occluding the femoral
artery, and then a small injection of thrombin to seal the
vessel. But there was a spill of thrombin into the femoral
artery, and the patient had to undergo peripheral thrombolysis
to reperfuse the lower extremity that was affected. So that
was one complication that had not occurred to me.
But then I had another complication
that really upset me: an infection of a Perclose suture. The
patient had to go through significant pain and suffering, had
to go for surgery, remained with chronic pain and had to receive
long-term intravenous antibiotic therapy to treat an infected
pseudoaneurysm.
It was then that I decided enough was enough!! I
had to find a safer way to deal with these patients.
|
|

Mauricio Cohen,
MD, FACC |
At the same time, I was enrolling patients
in a study looking at the pharmacokinetics of a IIb/IIIa agent
in morbidly obese patients
who weighed more than 275 pounds. Because I was very adamant about
enrolling patients in this study, I said, “I'm going to cath
all these large people who weigh more than 275 pounds.” So
then I decided that, if I'm going to cath them, I had better find
a safer way to do it.
So I refreshed the things I had learned initially in my training
in Argentina, and started to explore the different technologies for
access. I went through the process of teaching myself, and reading
throughout the literature on how to perform these techniques safely,
and what are the different challenges that you face. Then I attended
a transradial course by Dr. Tift Mann and that was very helpful.
Then I just started doing it.
Q: Did you have any problems initially
when you started using the transradial approach?
Dr. Cohen: It especially seems to happen in
this country, every time you introduce a new technique, or you say
you're going to do something new in the
cath lab, you start meeting resistance from the cath lab staff, because
some of them feel that it's slowing the flow of patients. Of course,
there's always a steep learning curve, and this curve has been very
well described for transradial access. So it takes time before you
find the optimal way of dealing with access, the optimal way of dealing
with different positions on the table, different way of sitting up
the table. But slowly, as I was getting more confident with the technique,
the staff in the cath lab and my peers started to realize that actually
transradial is a great technique, that patients have very few complications
related to access, that patients really enjoy it, especially those
who are morbidly obese, those who have significant back pain, or
who cannot lay flat for prolonged periods of time. And slowly what
started initially as just a clinical trial recruiting large patients,
granted me the referral from all my peers to do all large patients.
Q: So when they had obese or large patients, they sent them to you?
Dr. Cohen: They sent them to me. And then afterwards, after the trial
ended, the referring physicians and the patients were so happy
because of low incidence of complications and patient satisfaction,
that whenever a physician in our outpatient clinic decided to cath
a large patient, I would get an immediate referral for transradial.
Q: So initially you had learned it a little bit in Argentina?
Dr. Cohen: I'd seen it in Argentina. I’d always had it in the
back of my mind, and I was wondering why American physicians were
not doing it. At the same time you saw all the French, Canadians,
Spaniards and other people in the world that were huge fans of this
radial vascular access technique. And now everybody's coming to realize
that this may be the way to do cardiac catheterization in the future,
because you are avoiding bleeding outcomes that can actually take
the life of the patient.
The other thing for me was coming to realize that vascular closure
devices are far from ideal. They do not decrease the complication
rates. They decrease the time to patient ambulation, but they change
the nature of the complications. They are different complications.
That infected pseudoaneurysm, that really put a dent in my cath experience
and that prompted me to find a safer way to deal with vascular access.
Q: Do you have any tips and tricks to share?
Dr. Cohen: The trick is to have a good and supportive environment.
I think that doing your homework is very important, so you need
to read the literature, look at other peoples' complications and
have a good background reading.

Arm board
support for cath table |
|
Then I think it's very important
to have a comfortable set-up in the room, using a board. A good
support for the arm, a good support for your equipment by the
side of the table, is important -- using a board like we use
in our cath lab, and using adequate vascular access technology.
I think that the new short hydrophilic-coated sheaths, I'm using
an 0.21 wire, has made a difference to me, has facilitated access
significantly. Then people argue about the one-catheter versus
the two-catheter approach. The one-catheter approach with, for
example, a Kimny catheter or a multipurpose, is a little more
involved, and in the training program that didn't work as well
because in the end I always have to step in and manipulate the
catheter myself. |
So I think that the intermediate approach is to use Judkins catheters,
for example JR4 or 5 for the right coronary artery, and a JL3.5 for
the left coronary system. You always need to approach the easier
patients, start easy, with large, young and male patients because
they're more likely to have larger radial arteries and be complicated
less often with spasm. So if you start feeling comfortable, the way
I started with large patients who have large arteries, soon you will
be hoping to meet the challenge of doing normal-sized people, females,
then moving to older people who may have tortuosity in the subclavian
arteries and develop experience on how to navigate the difficulties
when accessing the supra-aortic vessels with the catheter.
Q: One of the objections I've heard is that you can't fit all different
kinds of equipment with radial access because of the smaller size
catheter.
Dr. Cohen: I think that's changing. It depends on the experience
of the operator. If the operator feels confident enough that he can
get all the difficult anatomy, including bypass patients with previous
CABG, it's up to the operator to decide that. So in many circumstances
you may not be able to do kissing stents or advance two stents into
the same vessel through the catheter, because you may need at least
a 7F catheter, or you may not be able to use a larger Rotablator
burr.
But the thing is, you do these procedures only in the minority of
patients. Most of the patients will be well served by a 6F catheter
and a simple intervention. And you can still do a kissing balloon
with a 6F approach. Here at UNC we have approached very challenging
anatomy and we have rotablators, rotational atherectomy, we have
complex bifurcation lesions, we have chronic total occlusions, and
it's a matter of feeling comfortable. I think that those fears are
just selected to a very small minority of patients, and in any case
there's no harm done by accessing the radial. You can always stage
the patient and bring them back and do transfemoral access.
Q: What about the other complication that sometimes occurs, which
is vessel spasm.
Dr. Cohen: Spasm has been one of the major complications initially,
when we did not understand very well or we did not have the right
equipment and we were in search for the right spasmolytic drug cocktail.
In my current practice, I only use 3 mgs of verapamil and I'm a little
bit cautious in patients with low ejection fraction. Other people
are using nitroglycerin, lidocaine and verapamil. Other people I
know are using other calcium channel blockers.
We do not see spasm as a significant complication, or a frequent
occurrence, at least in my practice. With the use of short hydrophilic-coated
sheaths, and small catheters, we can always overcome the problems.
When I approach patients, I always tell them that radial access is
usually more involved because you need a little bit more manipulation,
and in a certain number of patients they may experience pain as a
result of vasospasm. I tell the patients this is somewhat unpredictable.
But, if this happens during the case, the trade-off is that they
actually are able get up after the procedure and walk out of the
room, being able to be independent going to the bathroom and not
having to wait and lay flat for hours after a femoral sheath is pulled.
So I don't think radial spasm is that much of a significant problem.
Q: In terms of
fellowships its very important to introduce fellows to
this technique early on.
Dr. Cohen: Absolutely. Our interventional fellow that is
graduating this year, he's pretty proud about it. He's extremely
skilled and he has naturally good hands, but he's proud about
being able to go and offer this to the practice where he's going
to join.
This additional service to the patients he will be seeing,
I'm sure, will result in referrals specifically for him to
cath because he will be able to offer transradial access. |
|

University
of North Carolina
School of Medicine |
Q: It seems that the advantages are
so clear, more patient satisfaction, less bleeding – what
about nerve trauma in the femoral approach?
Dr. Cohen: Usually it goes away, but in a few cases it won't go away.
The beauty of doing transradial access is that there are no nerve
structures adjacent to the radial artery. The chance of injuring
a nerve structure is almost nil.
Q: You've made a tutorial slide show
about radial access. How do you use it?
Dr. Cohen: Actually, it's funny because in our cath
lab we have a significant turnover of staff. So every
day you turn your head
and you see a new tech or a new nurse. So every day was like starting
over again, and it was an endless job of training and teaching how
I want the table set, how I want the arm board set, and it was frustrating.
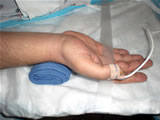
Click
to View Dr. Cohen's
Tutorial on Transradial
Access (Flash required) |
|
So I decided to
bring my camera, ask permission from the patient, and start
putting
together a short tutorial, so if the staff has a question, I
say go and look at my slideshow and if you have questions, ask
me.
I developed this slideshow
as an educational tool for the staff and also the fellows. And
the fellows like it. And I've been pleasantly surprised, because
every time I say now we're going to do radial, the fellows,
if they're not that familiar with the technique, they are able
to go online, look at the slides, and then they feel more confident
when scrubbing in the case. Sometimes when I like to challenge
them a little bit, I say did you look at my slides? So why are
you asking this question? |
The other thing that those slides help with
is the nurses in the cardiology unit. Because, at some point, patients
who had the radial
approach started to come back from the cath lab walking and going
to the bathroom. And the nurses were completely clueless. They had
always cared for patients who had had the femoral approach.
They knew that these patients needed to lie flat, could not get up,
or they’d be at risk for bleeding.
But then the radial patients started to come
with only these little bracelets on their hands! So the nurses
worked with me and we developed
an educational slideshow for them as well. We’ve also developed
a manual of policies and procedures in the cath lab.
Q: Thank you Dr. Cohen. We are making
your slideshow tutorial available online for
those interested in the details of the radial approach. Thank
you
again for
your time.
Dr. Cohen: You’re welcome.
This interview was conducted
in March 2008 by Burt Cohen of Angioplasty.Org; page last updated on
October 6, 2010
|







