![]()
<< To Homepage >>
<<Archives>>
February 2009 Archives: February 17, 2009 -- 5:00pm EST Medpedia -- OMG!!! According to Medpedia's founder:
Since the New York Times featured a screen shot of a page titled "Coronary Artery Angioplasty", I felt it was fair game to critique the information on the angioplasty page and its sister page on "Cardiac Stents". Cutting to the chase, I am far from impressed. In fact, I read these two pages and my reaction, as per the title of this posting, was OMG!!! If the information contained in these two entries is any indication of the accuracy of the rest of Medpedia, I would definitely advise patients to go elsewhere. The entries on angioplasty and stents are riddled with outdated and blatantly incorrect information about interventional treatments for coronary artery disease. I am truly surprised, given the sources that Mr. Currier cites in his statement to the New York Times:
It sounds impressive, to be sure, but here is just a sampling of the misinformation (with corrections) on the topic of angioplasty and stents: Medpedia states: "A heart attack occurs when blood flow through a coronary artery is completely blocked. Sometimes the accumulation of plaque causes the blood vessel to burst and a blood clot to form on the vessel surface." Bizarre to say the least. Arteries bursting?? This is not even close to a description of a heart attack. In describing an angioplasty, Medpedia states: "The doctor passes a long, thin, flexible tube (the catheter) through the sheath, over the guide wire, and up to the heart. The catheter is moved to the blockage, and the guide wire is removed." Perhaps this may be seen as wonkish, but the guide wire is NEVER removed during the procedure. It is the "rail" over which all catheters are advanced. It is only removed when the procedure is over and the patient is judged stable. In describing "cardiac stents", Medpedia states: "The meshwork of stents is usually made of metal, but sometimes a fabric is used. Fabric stents, also called stent grafts, are used in large arteries." Well...except that (1) "fabric stents" actually contain metal and (2) they have nothing whatsoever to do with coronary artery disease or cardiac stents -- stent grafts are used, sometimes, to treat a triple A -- Abdominal Aortic Aneurysm -- this is an unrelated medical issue which has nothing to do with blocked coronary arteries. Medpedia states that: "In about 20% of cardiac stent placements, the artery narrows again within six months of the angioplasty." Correction: with drug-eluting stents (DES), the numbers for restenosis are in the single digits. This is not news -- DES were introduced in the U.S. five years ago! Medpedia states that: "Treatment with radiation can also limit this growth [restenosis]. For this procedure, a doctor places a wire where the stent is placed. The wire releases radiation and stops cells around the stent from growing and blocking the artery. This procedure, involving intracoronary radiation, is known as brachytherapy." Unfortunately for Medpedia, not only has brachytherapy not been proven useful, but both companies making brachytherapy equipment ceased manufacturing several years ago. And I could go on, but I'll end with this...Medpedia states that "Metal stents preclude patients from having a magnetic resonance imaging (MRI) test within the first few months following the procedure." Except that the FDA approved both the Cypher and Taxus DES for immediate MRI FIVE YEARS AGO! In fact on Angioplasty.Org, we have a Patient Forum Topic just answering questions about this issue. Correction -- it is perfectly safe to have an MRI immediately following stent placement. As a rough estimate, it would seem that much of the information about interventional medicine on Medpedia is five years old. Angioplasty.Org has been online since 1997, has thousands of patient postings, and reports the most current news about stents, angioplasty and interventional medicine. Considering the quality of the information about this area that I've seen on Medpedia, I would not call it Web 2.0 -- rather Web minus 1.25. « permalink » « send comment » « back to top »
February 11, 2009 -- 12:25pm EST Taking Cost-Effectiveness to Heart
I'm all for expanding medical coverage: it's dis-heartening (sorry!) how many patients write into our Forum, unable to afford critical medications like Plavix because they've lost their insurance -- some have stopped taking it; some have had heart attacks as a result. So to expand coverage to more people, the money is going to have to come from somewhere. But my immediate reaction to hearing that government might be "comparing medical treatments" to determine which are "effective" is not so much the "I'm not going to let bureaucrats tell me what I can and can't do" stance, as it is the fact that, at least in the field of the treatment of heart disease, there are so many unresolved questions within the medical specialties themselves. And each new study or trial often (not always) adds new and confounding information. I mean we still aren't sure how long Plavix needs to be taken post stenting. Should we use bare-metal or drug-eluting stents, when and in whom -- or no stents at all because the Fractional Flow Reserve is above 80? CT Angiogram or not? Or should we reverse the historical trend and put interventions on the shelf, a la COURAGE, and stay with medical therapy only for most? If doctors can't agree on the best therapies, how can government agencies do so?
Personalized medicine. It's a concept that's been bandied about for a while now, but with new and exciting developments in decoding genetic markers, along with the hard work of physician teams and medical societies who have been authoring Appropriateness Criteria, the idea is being recognized as critical: a variety of available therapies is needed to treat a variety of individuals and physicians need to use the most current data to triage the right patients to the right therapy. Headlines in the popular press that proclaim "medical therapy trumps stents" or "CT scans are useless and costly" are meaningless, unless applied to specific patients with specific individual clinical situations. Stents or statins can be great for the right patient; not so much so for the wrong one. So, as someone who has never been able to walk into Macy's and just buy a suit off-the-rack, I sincerely hope the push towards cost-effectiveness does not put much stock in the concept of one-size-fits-all medicine.
« permalink » « send comment » « back to top »
February 6, 2009 -- 5:30pm EST Vote for Radial! We, at Angioplasty.Org, have been bringing this technique of catheter-based interventions to the forefront and now, theheart.org (part of WebMD) has taken up the question. The current voting is 47% to 53%, slightly favoring femoral -- but this almost 50/50 vote is interesting, since currently in the United States, only 3% of PCIs are done radially. If you favor the radial approach, let your voice be heard! « permalink » « send comment » « back to top »
February 5, 2009 -- 5:00pm EST CT Heart Scans, Radiation and the Media However, the point of this study was not to show that CT scans of the heart have suddenly been found to be dangerous! In fact, the doses recorded at the high end were what was considered "normal" less than a year ago (e.g. NY Times, June 29, 2008). Strikingly, as the accompanying editorial by Dr. Alfred Einstein states:
What is actually real important news, for both medical professionals and patients, is that, using dose reduction strategies, CT angiograms of excellent quality were done with exposures of only 2.1 mSv, approximately what New York City residents are exposed to annually, just from walking around. That's why I titled Angioplasty.Org's coverage, "CT Scans of the Heart Can Be Done with Low Radiation Dose." That's news!
For imaging professionals, the PROTECTION I study in JAMA has a clear message: learn the latest dose reduction strategies and work with your equipment vendor to implement them. With radiation at these low levels, CT angiography may mount a challenge to the most often-prescribed nuclear stress test, which carries radiation doses from 12-21 mSv. Of course, you never read headlines such as "Nuclear Stress Test Zaps Patients" because it's been around so long. Ever since multislice CT scanners became available in 2002-2003, industry and the imaging profession have been working on ways to reduce the radiation exposure. The PROTECTION I study in JAMA shows some positive results, but since 2007, when that data was collected, technology has advanced significantly -- enough so that Dr. Tony DeFrance, for example, regularly performs 320-slice scans with Toshiba's AquilionOne scanner at 1 or 2 mSv. Likewise, physicians such as Dr. Michael Poon are using GE Lightspeed units, and getting in similar ranges. Philips and Siemens have also developed low dose strategies. As evidenced at the start of this post, whenever a study about CT angiography is published, the popular press jumps on the story with accompanying "dreadlines", doing a disservice to the technology, those who practice it, and certainly to patients. A shining, and unfortunately rare, exception to this recent spate of news stories, was Dr. Nancy Snyderman, Chief Medical Correspondent for NBC News, who discussed her own CT heart scan with Matt Lauer on yesterday's "Today Show" (video below).
|
 So
yet another web-based health site was launched today, with great
fanfare in the
So
yet another web-based health site was launched today, with great
fanfare in the  Where
some insight can be found is in
Where
some insight can be found is in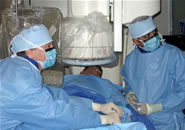 This
week's poll on theheart.org is about the transradial (wrist) approach
to catheterization and angioplasty. The question is "
This
week's poll on theheart.org is about the transradial (wrist) approach
to catheterization and angioplasty. The question is "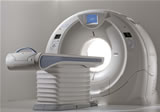 A
new study,
A
new study,  And
the implications for patients and professionals are profound. If
you are a patient, says Dr. Michael Poon, past president of the
And
the implications for patients and professionals are profound. If
you are a patient, says Dr. Michael Poon, past president of the