|
(1) An introduction to drug-eluting stents (also known as "drug coated stents", "medicated stents", or "DES"); (2) A history of drug-eluting stents, covering the evolution and mechanisms of these devices. For more in-depth information and late-breaking articles about drug-eluting stents, visit our Drug-Eluting Stent Center.
Part II. A History: Evolution, Development and Outlook for Drug-Eluting Stents
Since there was no interventional "fix" available, the only option for this patient was emergency bypass graft surgery to repair the problem.
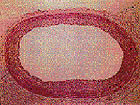
The Dilemma of Restenosis
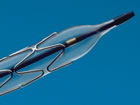
One such device was the stent -- a metal tube or "scaffold" that was inserted after balloon angioplasty. The stent itself was mounted on a balloon and could be opened once inside the coronary artery. Gary Roubin, Cesare Gianturco, Julio Palmaz and Richard Schatz were working on such stents in the United States; others in Europe were developing their own designs. In 1986, working in Toulouse, France, Jacques Puel and Ulrich Sigwart inserted the first stent into a human coronary artery. In 1993, the Gianturco-Roubin Flex-Stent became the first coronary stent approved for use in the United States, followed shortly by the Palmaz-Schatz. Over the next decade, several generations of bare metal stents were developed, with each succeeding one being more flexible and easier to deliver to the narrowing. A Persistent Problem
More and more, the solution moved away from the purely mechanical devices of the 90's and toward pharmacologic advances that were being made. If interventional medicine, using the body's circulatory system as a "highway" to deliver therapy, worked with devices, it could also work with medicines. Physicians and companies began testing a variety of drugs that were known to interrupt the biological processes that caused restenosis. Stents were coated with these drugs, sometimes imbedded in a thin polymer for time-release, and clinical trials were begun. "Stent Wars"
These newer drug-eluting stents have thinner, more flexible struts, thinner and more biocompatible polymers that elute the drug and, in most randomized clinical trials and observational studies, all show increased efficacy and safety: both the risks of stent thrombosis and the rate of restenosis have been reduced from the first generation devices.
Taking a different approach, Abbott currently sells in Europe (not yet available in the U.S.) a completely bioabsorable stent which will totally disappear after it has done its work. A number of other companies, such as Biosensors, Stentys, etc., also manufacture drug-eluting stents with different drug/polymer/stent combinations, but these also are not yet approved for use in the U.S. The major positive for drug-eluting stents is that all the approved devices have shown significant reduction of restenosis in clinical trials and in the "real world". DES have also shown dramatic reduction in reinterventions in diabetics as well -- this is a population that has been highly susceptible to restenosis in the past.
Late Stent Thrombosis The issue of late stent thrombosis, although discussed within the profession since drug-eluting stents were introduced, received widespread publicity at the September 2006 World Congress of Cardiology meeting in Barcelona when three European studies pointed to higher rates than had previously been seen (see our feature, "Problems Resurface with Drug-Eluting Stents" for detailed coverage). Late stent thrombosis was one of the major issues discussed at the 2006 TCT Meeting and the FDA scheduled a public meeting in early December 2006 on the issue. The conclusion was that more information was needed, especially about the use of devices in off-label settings, but that when used as directed, there did not seem to be greater risks of death or heart attack with drug-eluting stents. However, within a short time, newer second-generation drug-eluting stents came to market and studies have shown the risk of late stent thrombosis to be even lower. In fact the Swedish Stent Registry (SCAAR) which reported great concerns over stent thrombosis in 2006, has now shown the exact opposite, with drug-eluting stents showing far great safety and effectiveness than bare metal stents. Developments in this field can be fast and furious. Keep abreast of the constantly changing status of clinical trial results and controversies in our Drug-Eluting Stent NewsCenter.
The durability of interventional procedures to treat coronary artery disease non-surgically has increased exponentially with the introduction of drug-eluting stents. The specter of possible complications and the cost of repeat procedures is continually being reduced. And diabetics, a patient population that previously has not seen great success with interventional procedures, can now be treated with stents specifically approved for diabetics.
And so advances the story of interventional cardiology, started 40 years ago on a kitchen table....
Return to Part I. Drug-Eluting Stent Basics
Revised February 2013, Angioplasty.Org staff |