|
Fractional Flow Reserve
(FFR) Makes Stent Procedures More Cost Effective -- and Better!
|
 |
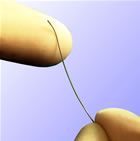
A type of
pressure wire, used to
measure
intracoronary
pressures
-- photo courtesy
Volcano
Corporation |
|
December
16, 2010 -- A report
in this week's Circulation, the Journal of
the American
Heart Association, analyzes
data from the highly-impactful FAME study and concludes:
"Economic evaluation of
the FAME study reveals that FFR-guided percutaneous coronary
intervention
in patients with multivessel coronary disease is one of those
rare situations in which a new technology not only improves
outcomes but also saves resources."
Angioplasty.Org has reported on the
FAME study since it was first presented
two years ago, but this new analysis details how fractional
flow reserve (FFR) is not only a better
way to guide
stent implantation, but a more cost-effective one, as well. |
Titled, "Economic
Evaluation of Fractional Flow Reserve-Guided
Percutaneous Coronary Intervention in Patients
With Multivessel Disease", the article uses data and one-year
outcomes from the FAME study to show that the mean cost of a stent procedure
(a.k.a. percutaneous coronary intervention or PCI) was reduced by almost $2,400
when decision-making was guided by FFR. The cost-savings come initially from
the reduction
in use of stents (1/3 less stents were used when FFR guided decision-making)
but continued through the first year, due to less need for repeat procedures,
re-hospitalization and adverse events. Two-year outcomes from FAME, although
not
included in this analysis, showed that the improved outcomes continued.
FAME: Fractional Flow Reserve Improves
Outcomes
The original FAME study looked at
a group of 1,005 patients with multivessel coronary artery disease
who were going to undergo stenting. The patients were randomized to
two
methods
for deciding which vessels and blockages needed treatment: (1) standard
angiography;
(2) standard
angiography
plus fractional flow reserve. Fractional flow reserve measures
the actual blood flow through the artery and in FAME, if the
blood flow was 80% of normal or less, the artery was stented, regardless
of how it appeared visually on the angiogram. For example, some blockages
looked worse on the angiogram than they measured with FFR, so for
these lesions, PCI was deferred and no stent was used.
Not only did the FFR-guided
cohort receive one-third less stents, but at one year the angiography-only
cohort had experienced a 39% increase in death, heart
attack or repeat procedures. The conclusion was not that stents were
ineffective,
but that stenting non-ischemic lesions offered no benefit. In
these cases, the complications and events associated with
stenting, even though small in percentage, were not offset
by any benefit, and therefore resulted in worse outcomes
overall. One conclusion that could be drawn from FAME was that the
use of fractional flow reserve made stenting safer,
as well
as
more effective. More about the original FAME study can be read in
Angioplasty.Org's exclusive
interview with Dr. Nico Pijls, the
study's principal investigator.
Fractional Flow Reserve is Not Only Cost-Effective,
But Cost-Saving
This week's study looked at all of the costs incurred by the FAME
patients, from the initial treatment decision-making in the catheterization
lab through the first year, including guiding catheters, regular
wires, pressure wires, balloon dilatation catheters, stents, antiplatelet
therapy, adenosine, contrast
media, and hospital days used for each patients index procedure. Added to this
were the costs associated with events that occurred during the first twelve months,
such as re-hospitalization, repeat stenting with or without incidence of heart
attack and subsequent coronary artery bypass grafting (CABG). The mean costs
per patient looking at this one-year period were $14,315 for the FFR-guided arm
versus $16,700 for the angiography-only arm: a cost-savings of $2,385 per patient.
Additionally, although
the
initial
procedure generated 90%
of
the total costs, the improvement
in patient outcomes throughout the first year in the FFR-arm led to
fewer
re-hospitalizations and
turned
out
to
be
a
significant
factor:
30%
of
the
total cost-savings.
Commenting on this outcome,
lead author, Dr. William Fearon wrote:
"It is unusual in modern medicine to find a new technology
or treatment strategy that not only improves the intended
health benefit and reduces risk and unintended effects but
also saves
costs....
A unique finding from the present analysis is the fact
that an
FFR-guided strategy to PCI in multivessel CAD not only
was cost-saving but also achieved these results in just 1
year,
a remarkably
short period of time.
Read Angioplasty.Org's exclusive
interview with Dr. Fearon for more information about how FFR is currently being used
at Stanford and other centers. |
|

William Fearon,
MD
Stanford Medical Center
|
Two additional cost items were identified by Angioplasty.Org:
one is the additional physician fee for placing the FFR wire, currently
around $100. Dr. Fearon told Angioplasty.Org that neither this fee
nor the physician fee for placing stents in an additional vessel
were included in their totals, since they were small and did not
become "significant" when the sensitivity analyses of varying the
costs
20% in either
direction were performed.
However, Dr. Fearon agreed that a second
item could potentially yield an additional cost-savings for
hospitals. Currently
total
reimbursement for stenting a single vessel is set by
Medicare at
one DRG (diagnosis related group) level. For multiple vessels,
Medicare pays a higher DRG reimbursement. However, that reimbursement
is fixed,
whether 2, 3 or 4 vessels or stents are used. So any
additional material or equipment costs must be absorbed by the
hospital. Dr. Fearon commented to us, "You are correct that the hospital
does
lose
money
if say
4 stents
are used instead of 2, for example. So in this respect FFR may
be advantageous to the hospital as well."
Usage of Fractional Flow
Reserve is Gaining
According to estimates, FFR currently is used in only 15%
of PCIs in the U.S. But that number is growing as more data is published
showing the clinical, and now the cost-savings advantages. Those
interventional cardiologists who do not use FFR
have previously pointed
to
the
fact
that it adds time to the procedure (3-5 minutes) and also costs
more (the pressure wire plus the drug adenosine, which is used during
FFR to
maximize
vasodilation, add about $1,000 in costs to the procedure). But,
as
Dr. Fearon points out in our
interview, with practice
the additional time becomes negligible. And this current study
on cost-effectiveness shows that the extra cost of equipment and
drugs
is more than compensated
for by the reduction in stenting and repeat procedures.
But more of a barrier
to the adoption of FFR is the perception by many
interventional cardiologists that a blockage they see with their
own eyes on the angiogram must be causing a problem for the patient
-- this is sometimes
called the "oculo-stenotic reflex":
if you see a blockage (a.k.a. stenosis), you must stent
it! Yet FAME showed that angiography is not accurate for diagnosing
whether
or
not a blockage is actually causing ischemia. In FAME two-thirds
of the blockages that measured 50-70% on the angiogram were
actually non-ischemic
and did not need stenting. Even in the most severe stenoses of
71-90%, nearly one out of five were not causing a problem, according
to FFR.
As for the clinical evidence that supports deferring stenting
on a lesion that is non-ischemic, after
two years only one of the 513
deferred lesions led to a heart attack (0.2%) -- and the improved
outcomes of the FFR-guided group remained intact.
About The Intravascular Imaging and Therapy
Center on Angioplasty.Org
To assist in educating the professional and patient population about
this new and evolving field, Angioplasty.Org created the "Intravascular
Imaging and Therapy Center" in 2007: a special
section devoted to information and news about intravascular ultrasound (IVUS),
optical coherence tomography (OCT), functional measurement and fractional flow
reserve (FFR) and future developments that can not only optimize interventional
treatment, but incorporate imaging and treatment in a single device.
The Intravascular Imaging and Therapy Center, supported by a grant from Volcano
Corporation, features overview articles about these techniques and interviews
with leading practitioners
in
the field,
such
as Drs. Antonio Colombo, Giulio
Guagliumi,
Augusto Pichard, William Fearon, Nico Pijls and Ron Waksman.
Reported by Burt Cohen, December 16, 2010
|



