A recent paper, published online before print in SCAI’s journal, Catheterization and Cardiovascular Interventions, yet again adds to the evidence that intravascular ultrasound (IVUS) imaging during PCI can improve stent placement and expansion in a way that may prevent stent thrombosis (ST).
Titled, “Angiographically confirmed stent thrombosis in contemporary practice: insights from intravascular ultrasound“, the study looked at five years (2005-2010) of a multicenter registry of stent thromboses and studied the IVUS images where performed.
Stent Under-Expansion: A Major Factor in ST
The result, not surprisingly, was that stent under-expansion was seen in 82% of all stent thromboses — but under-expansion was present in ALL of the early incidents of stent thrombosis (those happening shortly after stent placement). While the raw numbers are low, since stent thrombosis is a relatively low-frequency event, and IVUS use is unfortunately not as widespread as it could be, the data led to this conclusion from the Northern California research team:
There is a high prevalence of stent underexpansion in early ST, while the prevalence of malapposition is higher in very late ST. Use of IVUS during treatment for ST may identify mechanisms underlying the development of ST.
The authors also commented:
Prior studies have suggested that increased utilization of IVUS at the time of initial stent implantation increases the likelihood of adequate stent expansion and may decrease the rate of subsequent adverse cardiovascular events.
Stent thrombosis can be fatal 30-40% of the time, and is an event that has driven expanded use of expensive antiplatelet therapy. Is it possible that a significant number of these events, specifically the early ones, could be prevented, or at least better treated, through the use of an imaging technology that’s been around for more than two decades?
Revisiting Early Lessons About Causes of Stent Thrombosis
I’ve written about this issue before. And so have many interventional cardiologists in many peer reviewed journal articles, starting with Dr. Antonio Colombo, all the way back at the beginning of the stent era in the early 90’s.

Antonio Colombo, MD
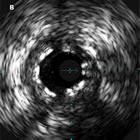
When stents first came on the scene, Dr. Antonio Colombo became concerned about the high incidence of blood clots inside these early bare metal stents, and he started using what was then a relatively new imaging modality, intravascular ultrasound, in order to get a cross-sectional view of the stented artery. What he found was what similar to the IVUS image at the top of this article: many stents were being significantly under-expanded (the white ringed area near the center of the image is the stent, with an area of 4.2 mm2, but the IVUS image shows the vessel to have a 6.8 mm2 area).
I asked Dr. Colombo how stent under-expansion causes problems in one of the first interviews I conducted to launch our Intravascular Guidance Center back in 2007, and he told me:
You have a stent which is in a less optimal contact with the vessel wall. You have more turbulence. You have struts that are not perfectly attached or embedded in the plaque, and you may have more foreign body protruding into the lumen, increasing the risk of restenosis and thrombosis.
High-Pressure Deployment and Accurate Measurements
Colombo’s findings led to the era of high-pressure balloon deployment of stents, and the stent thrombosis rate dropped significantly. But it still exists. And in the era of drug-eluting stents, it’s been thought that the use of high-pressure deployment may not be as necessary.
This brings us back to the image at the top of this article. It’s not from the early 90’s — it’s a recent drug-eluting stent example from the C&CI paper!
I often use the example of fitting a window or door into the wall of a house. You have to measure the opening very carefully so the frame fits snugly and keeps out rain, wind, cold. Measuring the diameter of a moving coronary artery using angiography alone is just not accurate enough, because you’re seeing what Dr. Gary Mintz calls a “silhouette-o-gram” which can hide disease. You try to measure the diameter of the shadow of an artery, and you can’t see what’s arterial and what’s plaque. With IVUS, you can see several layers deep into the vessel wall, and very accurately characterize the anatomy and measure the actual vessel wall.
Additionally, and very important in terms of safety and confidence, by knowing that the vessel diameter is X, you have the confidence to fully expand the stent without over-expanding the vessel and causing a dissection, especially if you see calcium deposits on the IVUS.
Why Isn’t IVUS Routinely Used in the U.S.?
There may never be a randomized clinical trial which will be able to show that using IVUS (or possibly a newer technology, OCT) will reduce the incidence of stent thrombosis but, as in the recent C&CI study, anecdotal and registry evidence is clearly there.
The problem is, of course, one of money. Yes, using an IVUS catheter adds to the immediate cost of the procedure, and a minimal amount of time. But if readmissions, or even mortality, can be reduced by using a technology that allows more accuracy in stent placement and expansion, isn’t that cost-effectiveness?
The Japanese feel this way. Unlike in the U.S., where IVUS penetration is about 15-20% or so, IVUS is fully reimbursed in Japan and is very widely utilized. And the results of several major drug-eluting stent trials reveal an interesting factoid: the Japanese arm of the trial always seems to have better results, better outcomes.
When I asked Dr. Shigeru Saito, the principal investigator in Japan for many major stent trials, including Xience and Endeavor, why this was so, he answered in one word: IVUS!
You can read more of his comments and others about how IVUS can reduce complications and improve outcomes in our article, “Intravascular Ultrasound (IVUS) Use Growing with Integration into Routine Cath Lab Imaging” and in many other articles and interviews throughout our Intravascular Guidance Center.