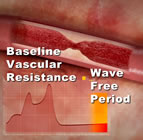
Angioplasty balloon being manufactured on the kitchen table in Gruentzig’s apartment
Today is the 35th anniversary of the first percutaneous transluminal coronary angioplasty (PTCA) which was performed in 1977 by Dr. Andreas R. Gruentzig in Zurich, Switzerland. This angioplasty procedure utilized an expandable balloon, fashioned on a kitchen table in Gruentzig’s apartment by Gruentzig’s assistant, Maria Schlumpf (note the bottle of wine…and yes, she used Krazy Glue).
The patient was Adolph Bachman, age 37 (the same age as Gruentzig), who was scheduled for bypass surgery. Gruentzig has been working on this idea for several years; it was an idea first germinated by a U.S. radiologist, Dr. Charles Dotter, in the early 60’s. Dotter in fact coined the term “angioplasty” to describe opening up a blocked artery not through open surgery, but by threading a catheter into the artery and opening it up from the inside out: less traumatic, quicker, and possibly (he thought) more durable.
Dotter’s idea was mocked as crazy (he became known as “Crazy Charlie”) by the surgical community of the day and it took years for Dotter’s concept to travel across the world to Europe, where Gruentzig learned about it. He added a balloon to the tip of the catheter and, after experimenting in the lab in Zurich, he teamed up with Dr. Richard K. Myler of San Francisco to try the idea intraoperatively in patients who were having open heart surgery.
When the concept had been proven in a few of these surgical cases, Gruentzig returned to Zurich to attempt doing an angioplasty in the cath lab without surgery: percutaneously — just through a needle stick, the same procedure as a diagnostic angiogram. Except with a balloon. That’s where our video below begins: the story of the first angioplasty.
(By the way, the clip below is excerpted from my feature-length award-winning documentary, “PTCA: A History,” which tells the whole tale of how this “crazy” idea turned into a major branch of modern medicine. The complete 72 minute DVD is available for sale on our web site — of course!)
Continue reading →

 Published “online first” today in the New England Journal of Medicine are two articles, authored by the Democratic and Republican presidential nominees, President Barack Obama and former Massachusetts Governor Mitt Romney, describing their health care platforms and their visions for the future of American health care. The editors of NEJM had asked the nominees for these statements which are brief and concise, summing up the two positions in less than 1,300 words each.
Published “online first” today in the New England Journal of Medicine are two articles, authored by the Democratic and Republican presidential nominees, President Barack Obama and former Massachusetts Governor Mitt Romney, describing their health care platforms and their visions for the future of American health care. The editors of NEJM had asked the nominees for these statements which are brief and concise, summing up the two positions in less than 1,300 words each. Findings in a
Findings in a

 A study from Denmark of almost 100,000 patients over a 12-year period has concluded that:
A study from Denmark of almost 100,000 patients over a 12-year period has concluded that: