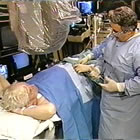
Cardiologist talks to a patient “on the table” in cath lab
Something that is “on the table” is defined as an item that is “up for discussion.” And this week The Society for Cardiac Angiography and Interventions (SCAI) issued a consensus statement about the proper use of “ad hoc PCI” — and the patient was definitely on the table, up for discussion, part of the conversation.
Since we’re into definitions, ad hoc PCI is the scenario in which a diagnostic catheterization is followed in the same session by PCI (angioplasty and stents). And this is a common scenario: in New York State, for example, 80% of all angioplasties are done in the same session as the diagnostic angiogram, although the vast majority of these are emergency or primary angioplasties, where a patient in the midst of a heart attack (or close to it) is brought into the cath lab and the blockage is opened up, saving the heart muscle and possibly the patient’s life.
There’s no question or debate that emergency PCI should be performed this way; the question is whether and when it is appropriate to perform an elective intervention on a stable patient immediately after the angiogram.
This didn’t used to be a question. “Back in the day”, when angioplasty was in its first decade, ad hoc PCI was most definitely not the order of the day.
At that time there were no stents: angioplasty was done with a balloon only (today called POBA or “plain old balloon angioplasty” — cute, huh?). The problem was that sometimes after the balloon was inflated and the blockage opened, the coronary artery collapsed . Sometimes a balloon could be re-inflated to keep it open, but 3-5% of the time the patient had to go to emergency surgery to repair/bypass the collapsed artery: a pretty traumatic ending to what was supposed to be a minimally invasive procedure!
So understandably, given the risk of abrupt closure, a diagnostic catheterization was done, the patient was sent to the recovery room, and the x-ray films were studied, often by a team of physicians.

Robert Harrington, MD
As Dr. Robert Harrington, Chief of Medicine at Stanford University, describes:
“Every patient case became a rather detailed discussion around what was best. And remember the days of cath conferences where there would be much discussion and even heated debate amongst interventional cardiologists, non-invasive cardiologists and our surgical colleagues about what might be the appropriate approach for that particular patient.”
Then came stents: metal scaffolds that had the ability to hold the artery open after the balloon inflation. Soon the complications of angioplasty that resulted in emergency bypass surgery became one in a thousand or less. The procedure became much safer. So much so that it became feasible, even desirable, to add another 30 minutes or so onto the diagnostic procedure and open up the blockage. One stop shopping…or stenting: ad hoc angioplasty!
What was gained was efficiency, less patient discomfort, lower costs…what was lost was that period of decision-making, of debate about the best way forward.
And, as Dr. Harrington relates:
“As we moved from an era of balloon angioplasty to an era of stenting and other improvements in the technology, as well as the concomitant medical therapies, in many ways the procedure became technically less difficult. And because of that we moved into this era of ad hoc procedures for much of what we did. But in a credit to the community, evidence continued to be accrued both observational and in randomized trials and now we’re having the interventional community step back and say, ‘You know, it’s not just a simple this or that decision.’ It is more of a series of decisions that involve understanding the patient demographics, understanding the patient’s coronary anatomy and cardiac function, and importantly understanding what the patient thinks about the whole thing, because there are some trade-offs in choices.”
Dr. Harrington is talking about the COURAGE trial which showed that, in some cases, the option of modern medical therapy might now equal the outcomes of angioplasty — although angioplasty relieved symptoms of angina more quickly. Or SYNTAX, or more recently FREEDOM, which showed that some very complex coronary disease might be better treated with bypass surgery — although the surgery carried a small increased risk of stroke. Or FAME and FAME 2, which showed that just because a blockage looks obstructive on the angiogram doesn’t necessarily mean it is — using fractional flow reserve (FFR) can help decide whether or not the stenosis needs opening. Not simple choices.
But perhaps now, it’s “Back to the Future”: back to the era of debate and discussion before dilation — at least in some cases. Maybe don’t go straight ahead and open up those blockages. Instead open up a discussion about the best therapy, as Drs. Nallamothu and Krumholz suggested in their 2010 editorial in JAMA, “Putting Ad Hoc PCI on Pause.”
And…put the patient on the table. Not the cath lab table, but the discussion table. The recent revision of the Guideline for the Diagnosis and Management of Patients With Stable Ischemic Heart Disease contains an entire section, titled “Vital Importance of Involvement by an Informed Patient,” and it’s a Class I recommendation. Cardiologists need to engage in a discussion with their patients, find out the patient’s preferences, explain the various possible courses of action, what the risks and benefits of each are, and come to an agreement that respects the patient’s choice while ensuring the patient’s safety.
Andreas Gruentzig and patient
As I wrote back in September in “An Informed Patient is a Healthier Patient,” when Andreas Gruentzig first began performing angioplasty, he carefully explained what he was planning to do and was realistic about what the patient might expect, both on the cath lab table and afterwards, in terms of outcomes. As Adolph Bachman, the very first coronary angioplasty patient, said to me:
“Everything was so clear. Even as a total layman, I understood his method. I understood what was going to go on and I knew there was no reason to worry. I was 100% convinced that it would be successful. But that was all because Dr. Gruentzig was so clear and because the method itself was so simple.”
As angioplasty has gotten more sophisticated and is now able to address a much wider spectrum of coronary disease, those explanations might not be as simple as they were back in 1977. But the more physicians and patients are able to talk to each other, the better the outcomes will be.
Of course, as Dr. Harrington discusses in our report on the SCAI Consensus Statement, someone is going to have to figure out how to reimburse for these discussions. But that’s another story…to be continued….




I wish to congratulate Dr. Robert Harrington, Chief of Medicine at Stanford University,for his clear and succinct observation and word of wisdom. Yes indeed open up the crucial discussion before opening up the culprit artery and also open up further discussion and advice after achieving the desired perfusion and perfection. With Warm Regards
Dr V P Nair, MD, FRCP, FACC, FESC FAPSIC, Cardiologist, Mt Elizabeth Medical Centre, Singapore
I recently received an Ad Hoc stent in my Circumflex Artery without any knowledge that a stent was a possibility. I had between 70% and 80% blockage and we never discussed a stent prior to my cardiologist’s “lets take a look-see” heart cath.
I wish that I had discovered this site two weeks ago because I would have told my cardiologist that if any blockage was discovered and it wasn’t an immediate threat to my life, I didn’t want it done until we could take a step back and discuss other options.
Great Article!!!!