Best medical practices for angioplasty and stent placement are a moving target because no sooner than a guideline is published it can be changed by the results of a more recent study. And the SCAI Ad Hoc PCI Consensus Statement posted online just three days ago is no exception.
In fact the very first decision point for a patient with stable ischemic heart disease may now be modified (at least for some interventional cardiologists) by the results of the FAME 2 study. As Dr. James Blankenship, lead author of the SCAI paper, told Angioplasty.Org, “[This statement] was written and accepted for publication before the FAME 2 results came out.”
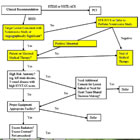
Briefly stated the flow chart, published online in Catheterization and Cardiovascular Interventions, indicates that when a diagnostic angiogram reveals a significant blockage, or a blockage that is not consistent with a noninvasive study (a stress test that hopefully was done before the angiogram was ordered), then it is reasonable to perform an FFR (Fractional Flow Reserve) study while the patient is on the table. This takes just a few minutes and measures the actual coronary blood flow across the blockage or lesion that is seen on the angiogram.
If the FFR study is positive or abnormal (i.e. more than 20% of the blood flow is being restricted), the flow chart then asks whether the patient has been given a course of maximal medical therapy to control the angina. If not, the flow chart suggests that the patient be taken off the table and prescribed a course of optimal medical therapy (OMT). If the patient already has tried the medical therapy option, then the flow chart recommends proceeding down the pathway towards ad hoc angioplasty.
However, the results of FAME 2 showed that patients with stable ischemic coronary disease who had a positive FFR test are best treated with PCI immediately. In fact the FAME 2 trial was halted prematurely on ethical grounds because patients who were ischemic and who were randomized to medical therapy had a significantly higher incidence of “urgent revascularization.”

James Blankenship, MD
I asked Dr. James Blankenship, the lead author of the SCAI Consensus Statement, about this and his response was:
“Based on FAME 2, one could argue that our algorithm is on the conservative side. Of course, this was written and accepted for publication before the FAME 2 results came out, so the next question might be ‘Does FAME 2 render this strategy obsolete?’ I think when you look at FAME 2, if you’re a proponent of PCI and doing it aggressively, then one could say, ‘Yeah this is obsolete. Forget the trial of maximal medical therapy.'”
Certainly the proponents of OMT over PCI would stress trying medical therapy first. As for Dr. Blankenship, here’s his assessment of Fractional Flow Reserve (FFR) :
I think that FAME and FAME 2 certainly have increased and will continue to increase the use of FFR. Our lab has found it to be an extraordinarily valuable tool for making on the spot decisions. I think that one of the biggest changes we’ll see in practice will be more increase in the use of FFR and I think that will significantly improve the quality of care that we deliver to our patients: in some cases preventing coronary interventions that perhaps weren’t necessary and in some cases helping you do them in cases where you might not otherwise. Because clearly there are some lesions where I take a look at it and say, “Nah, that can’t possibly be significant.” But you put a wire across it and darned if it isn’t. And then we end up fixing it. And conversely there’s some where you suspect that it’s significant but turns out not to be and then you’ve saved the patient an unnecessary procedure. So I think that FFR will prove to be an invaluable tool increasingly in the future.
‘Nuff said….




Well said. The benefit of FFR should be obvious to all interventionalists by now. If you’re an interventionalist and not using FFR you are practicing old medicine and should consider retooling or retiring.
Thanks! FYI, Morton J. Kern, MD, FSCAI, FAHA, FACC is Chief of Cardiology Long Beach VA and Associate Chief Cardiology UC Irvine School of Medicine.